Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
Every time you shower or brush your hair, it seems like more and more hair is falling off your head. What could be causing this hair shedding?
Losing a certain amount of hair every day is normal, but if you’re losing a lot and seeing noticeable changes in hair loss, all that hair in the shower drain might be causing you tremendous stress.
Here’s the good news: hair shedding is different from male or female pattern baldness. It’s usually a short-term condition that will go away. Here’s a look at how to tell if your hair shedding is excessive, what could be causing this issue, and what you can do about it.
What is hair shedding?
Hair shedding occurs when your scalp hair follicles prematurely change from the growing phase to the resting phase of the hair growth cycle, which ends with the hair falling out. The medical term for this is telogen effluvium (Bergfeld, 2001).
The hair cycle has three phases (Al Aboud, 2020):
The growth phase or anagen phase—this is where 90% of hair is at any moment
The resting phase or catagen phase, where the hair stops growing
The shedding phase or telogen phase, where the hair falls out
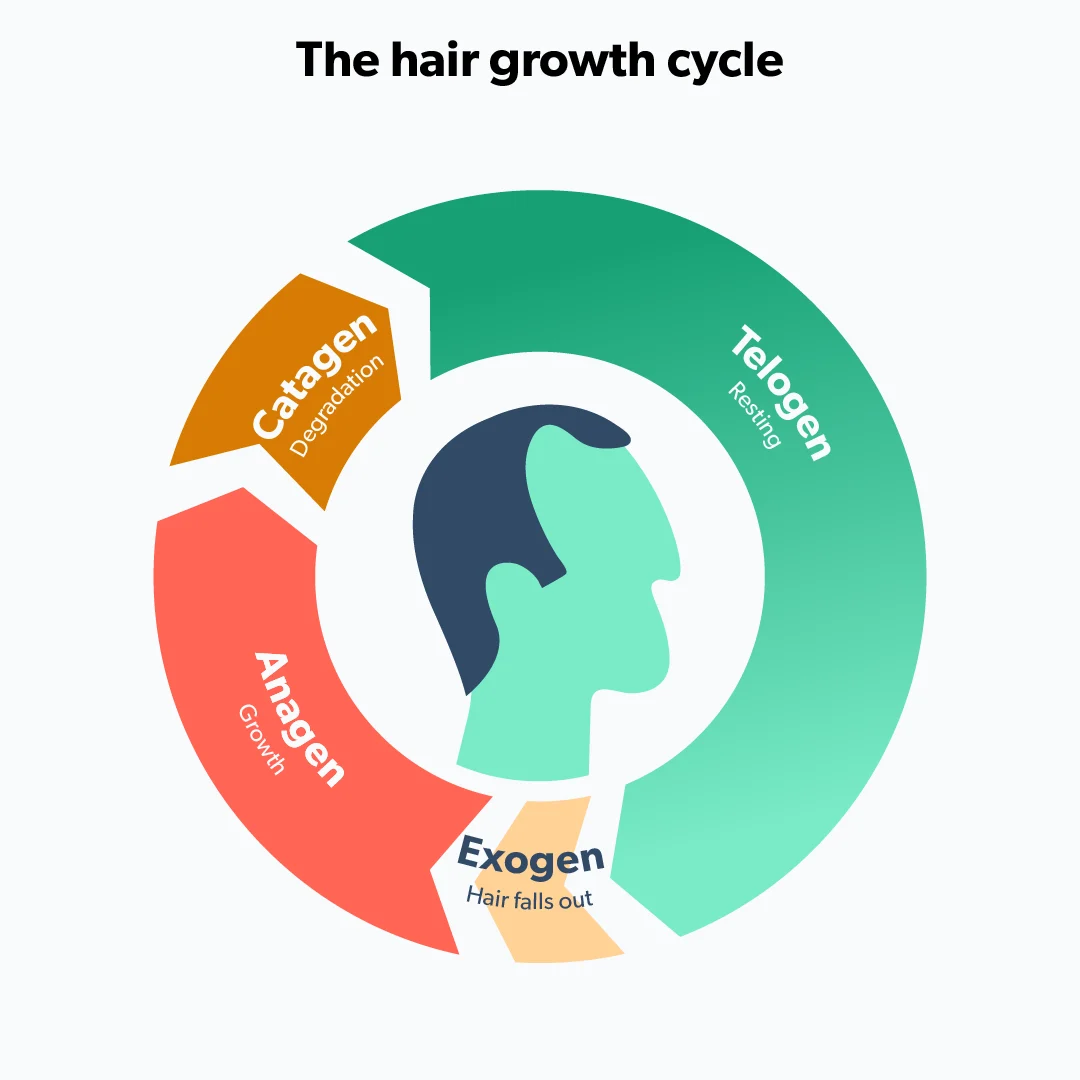
While some hair thinning is expected, in telogen effluvium more hair than usual enters the resting and shedding phases (Hughes, 2021).
Episodes of increased hair shedding can occur in people of any age, any gender, and any racial background. Researchers don’t know precisely how often it happens, but it‘s thought to be quite common. A large portion of adults will experience an episode of telogen effluvium at some point in their lives (Hughes, 2021).
Many women are more likely to experience hair shedding since one frequent cause is hormonal changes after giving birth and other points in their lives (Hughes, 2021).
When is hair shedding excessive?
Since about 10% of your hair follicles are in the resting or shedding phases at any given time, you naturally lose some hair each day. Researchers estimate that people lose an average of 50–150 hairs over a 24‐hour period (Kovacevic, 2017).
If you’re worried that you’re losing too much hair, a simple way to check is with the Hair Pull Test. This should be performed on dry hair when you haven't shampooed for at least 24 hours. It can help you determine the severity and the location of the hair loss (Mubki, 2014).
Grasp 50 to 60 hairs between your thumb, index, and middle fingers.
Pull firmly but gently away from the scalp and along the hair shafts.
Repeat this test on four different regions of the scalp (for example: near the hairline, the crown, and on either side of the head).
Count the number of hair strands that came loose with each pull.
Pulling more than 5–6 hairs in a section is considered a positive hair pull test. This means you likely have active hair shedding in that area and may have telogen effluvium (Mubki, 2014).
What causes excessive hair shedding?
Excessive hair shedding is usually an acute reaction to some form of stress on the body. An episode usually lasts less than six months and is often much shorter. Typically looking at your medical history will reveal a cause that occurred between one and six months before you noticed the shedding (Hughes, 2021).
You might have even fully recovered from whatever initially caused your hair shedding, and the shedding is a very delayed effect. This can sometimes make it difficult to see the connection with your hair loss. Some common causes of excessive hair shedding are listed below (Hughes, 2021).
Medical conditions
Many medical conditions can lead to hair shedding. Common triggering events include (Hughes, 2021; Bergfeld, 2001):
Acute fever
Severe infection
Major surgery
Thyroid disease
Heavy metal ingestion
Iron deficiency
Autoimmune diseases such as lupus
Kidney or liver disease
Chronic infections such as syphilis
Certain medications
Excessive hair shedding is a possible side effect of several different types of medications. The most common types of drugs that can cause hair loss include (Hughes, 2021):
Beta-blockers
Retinoids
Anticoagulants
Propylthiouracil
Carbamazepine
Immunizations
Hormone changes
Women are more likely to experience hair shedding due to changes in their hormones throughout life. This can be caused by (Hughes, 2021; Bergfeld, 2001):
Heavy periods that can lead to iron deficiency
Starting or stopping hormonal birth control
Recent pregnancy or miscarriage
Any condition that causes a decrease in estrogen levels
Polycystic ovarian syndrome (PCOS)
Menopause
Diet
A lack of adequate iron or protein in your diet or sudden weight loss can all contribute to excess hair loss. Telogen effluvium is a common symptom of eating disorders as well. Studies have shown that 67% of patients with bulimia and 61% of patients with anorexia nervosa experience hair shedding (Mubki, 2014).
The correct balance of vitamins and minerals is essential for healthy hair growth. Correcting low levels of vitamin D, iron, and vitamin C can improve symptoms of hair loss. On the other hand, studies have shown that taking too much Vitamin A or selenium can increase your hair loss (Almohanna, 2019).
Mental stress
Mental health disturbances such as acute anxiety or depression have been known to lead to hair shedding. Severe life stressors such as the death of a loved one, the end of a relationship, or financial difficulties may also result in increased hair loss (Mubki, 2014).
How to stop hair shedding
Sudden episodes of hair shedding are typically short-lived and will clear up on their own. Your normal hair will return a few months after the stressful event has ended, usually without any treatment (Hughes, 2021).
Treat the cause
If your hair shedding was caused by a hormone or dietary imbalance, metabolic disorder, or chronic infection, you’ll start seeing new hair growth after correcting these issues. If your hair loss is due to medication, ask your healthcare provider if there are alternatives you can take. Hair growth will restart after you stop the drug (Hughes, 2021).
Medications
Medications aren’t usually needed for hair shedding but can be considered in severe cases. Topical minoxidil (Rogaine) hasn’t been proven to promote hair growth in telogen effluvium. However, it has helped with hair regrowth in other conditions. (Hughes, 2021).
When to see a healthcare provider
For the most part, you usually don’t need to see a healthcare provider about hair shedding. It typically lasts only a few months and stops on its own. There are some exceptions, though.
If you experience a sudden increase in the amount of hair you are shedding without an apparent cause, you should contact your healthcare provider. You may have an underlying medical condition that needs to be treated (Hughes, 2021).
You should also see a healthcare provider if you start to lose hair on other parts of your body besides your head or your hair loss is concentrated in specific spots. These aren’t common symptoms of hair shedding and may indicate a different condition (Hughes, 2021).
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
References
Al Aboud AM, Zito PM. (2020). Alopecia. [Updated 2020 Sep 29]. In: StatPearls [Internet]. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK538178/
Almohanna, H. M., Ahmed, A. A., Tsatalis, J. P., & Tosti, A. (2019). The role of vitamins and minerals in hair loss: a review. Dermatology and Therapy, 9 (1), 51–70. doi: 10.1007/s13555-018-0278-6. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6380979/
Bergfeld, W. F., & Mulinari-Brenner, F. (2001). Shedding: how to manage a common cause of hair loss. Cleveland Clinic Journal of Medicine, 68 (3) 256-261. Retrieved from https://www.ccjm.org/content/68/3/256.long
Hughes EC, Saleh D. (2021). Telogen effluvium. [Updated 2021 Jun 8]. In: StatPearls [Internet]. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK430848/
Kovacevic, M., Goren, A., Shapiro, J., Sinclair, R., Lonky, N. M., Situm, et al. (2017). Prevalence of hair shedding among women. Dermatologic Therapy, 30 (1), e12415. doi: 10.1111/dth.12415. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6175177/
Mubki, T., Rudnicka, L., Olszewska, M., & Shapiro, J. (2014). Evaluation and diagnosis of the hair loss patient: part i. history and clinical examination. Journal of the American Academy of Dermatology, 71 (3), 415.e1-415.e15. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S0190962214014364?casa_token=XwOdKExAbgsAAAAA%3ABGXU1Ex3iWqb1p9Ug6y8ikoVsnwzRn9Ba511RZsHDe3Fpyrs8nmyGhXVs2gS0fHX57vG0avFAQeU












