Insurance
Join thousands of Ro weight loss patients
How insurance works with the Ro Body membership
We know insurance can be a headache, which is why we have a dedicated concierge who will work to find you insurance coverage for medication. But how does it all work and how long will it take? Let’s get into it!
We help you lose weight by pairing revolutionary medication with coaching, care, and healthy lifestyle changes to make it last.
The cost of medication is not included in the monthly membership fee.
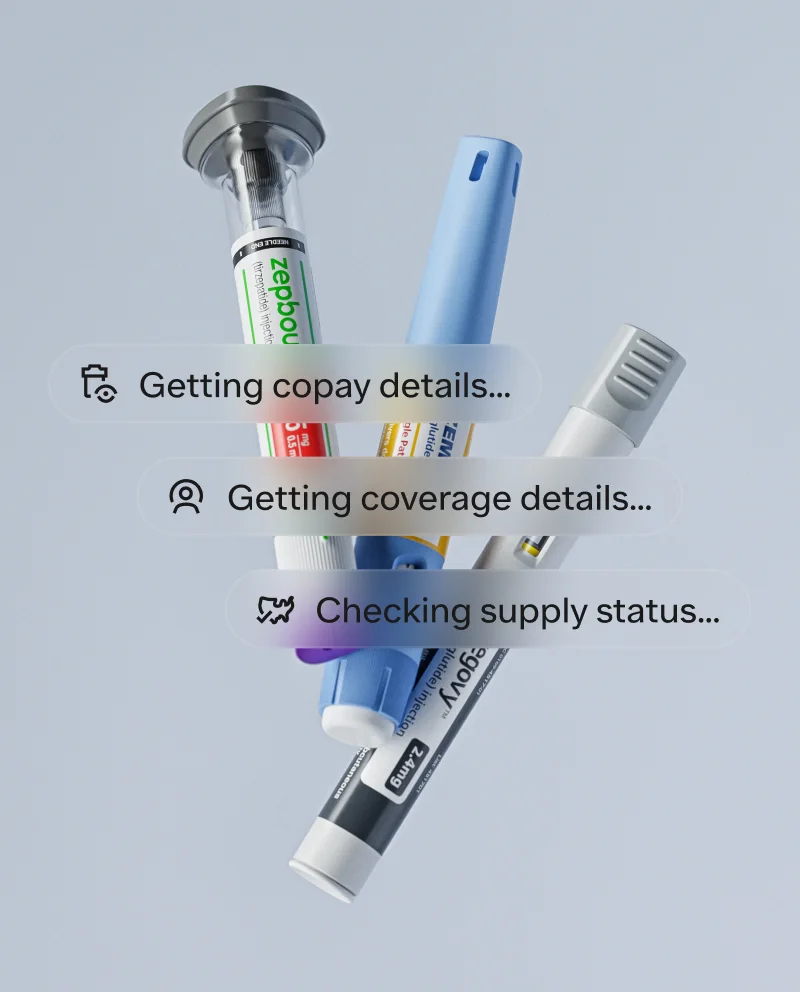

When you get approved, our partner goes to work
You’re approved for treatment, now what?
If a Ro-affiliated provider writes you a prescription, our concierge will coordinate with your insurance to help get medication costs covered. They'll verify your benefits and handle any paperwork (including submitting for prior authorization, if needed). It typically takes between 1-3 weeks. When coverage is determined, our concierge will send your prescription to your pharmacy to be filled.


Here’s how our insurance concierge gets you covered and finds medication

Liaise with your insurance
They'll take care of communicating with your insurance company, and even handle the paperwork.
Find solutions to get you started
If your provider writes you another prescription, our concierge will work with your insurer to try and get it covered. If all attempts fail, we'll walk you through cash payment options.
Explore medication options
If your insurance denies one medication, your provider may recommend another option for you.
Send your prescription to your pharmacy
If your pharmacy doesn't have medication due to national shortages, you'll join their waitlist, and our concierge will contact your pharmacy periodically to check on your prescription.
Your timeline to treatment
From personalized treatment to insurance support, we help you get—and stay—on track.
Start losing weight in 5 simple steps
1. Start your online visit
Answer a few questions about your health and goals, all online—no in-person doctor’s office visit necessary. You’ll find out if you’re eligible within 2 days.

2. Provider writes an Rx (if appropriate)
A provider will review your info and prescribe the right GLP-1 treatment for you, if eligible. Get ready for your first dose in two weeks if using insurance, or less than a week if paying cash.

3. Check your insurance coverage
Ro checks your insurance to see if GLP-1 coverage is available. If you require prior authorization, Ro's insurance concierge fights for coverage and submits all paperwork on your behalf. If you're covered, a prescription is sent to your pharmacy. If not, your provider will suggest alternative FDA-approved cash pay GLP-1 options. This process takes about 2-3 weeks.

4. Start your treatment
If paying cash, your medication ships right to your door and you can take your first dose in less than a week. If using insurance, your medication can be picked up at your pharmacy.
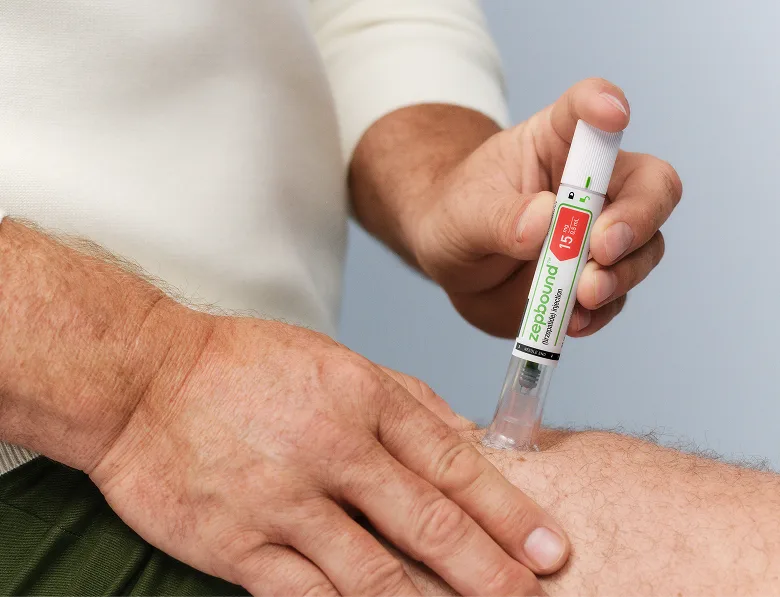
5. Get support to stay on track
Keep making progress with regular check-ins, expert guidance, and access to your care team 24/7. Ongoing care and support is there for you when you need it—whether it’s a quick chat with your provider or routine check-ins, we’re with you every step of the way.
Insurance 101
Can I use insurance with Ro?
If you want to use insurance to pay for GLP-1 medication, Ro will be there to help you navigate your coverage! As part of the Ro Body membership, you’ll get access to our insurance concierge who will:
work directly with your insurance provider to check if your medication is covered
handle any paperwork and coordination for you
When it comes to navigating insurance coverage, you don’t have to lift a finger. And if you're covered, you may just have a monthly copay for the medication depending on your plan. You’ll pay the pharmacy directly for your medication.
Please keep in mind: Insurance does not cover the cost of the Ro Body membership. Additionally, GLP-1 medication is not included in the cost of membership and is billed separately. Some medications offered through Ro are cash-pay only, meaning we cannot offer insurance concierge services for those options.
What if my insurance doesn’t cover the medication?
If for some reason your insurance will not cover the cost of your medication, you’ll have the option to either select from cash pay medication options or you can cancel your Ro Body membership at any time.
How much do GLP-1s cost?
How much do GLP-1s cost? Costs vary based on medication and dose, whether you use insurance or pay cash, and if you choose Prepay & Save.
Using insurance? Our insurance concierge fights for coverage—which means your medication cost might just be your copay.
Paying cash? You have access to the lowest-price GLP-1s—at the same prices as LillyDirect®, NovoCare®, and TrumpRx. Options start at $149/month* and increases for higher doses.
On Ro, Prepay & Save can unlock even more savings.
*For a limited time, new patients can start on the lower doses of Wegovy pill for $149/mo
Additional Ro Body membership fee required. The Ro Body membership fee is as low as $74/month when you prepay on an annual plan.
How does getting insurance coverage for medication work?
The first step is to study the fine print of your current plan. Our insurance concierge reviews it to see if your GLP-1 costs can be covered without prior authorization (specific approval from your insurance company to cover your medication). This is the benefits verification stage, and at this point, nothing has been submitted to your insurance.
If the fine print doesn’t show automatic coverage for your GLP-1 medication, the next step is to submit a prior authorization request to your insurance company. Prior authorization is a decision by your health insurer that your medication is medically necessary. This allows your insurer to evaluate if the treatment is covered as a plan benefit (and if they can assist with payment).
It can be a complicated process that varies by insurer. That’s why we work with our insurance concierge to do the hard work of gathering your information, submitting your prior authorization request, and going back and forth with your insurance company.
How long does the review take?
It can take about 2–9 days, but once your insurer reviews the request, there are a few possible outcomes:
Approved with co-pay
Approved with no co-pay
Denied
What is prior authorization?
Prior authorization is a decision by your health insurer or plan that a health care service, treatment plan, or prescription drug is medically necessary. In our case, prior authorizations allow your insurance company to evaluate if a GLP-1 medication is covered.
The process for obtaining prior authorization varies by insurer, but involves submission of administrative and clinical information by the treating practitioner. Behind the scenes, our insurance concierge partner does the hard work of gathering your information, submitting your prior authorization request, and going back and forth with your insurance company.
How long does prior authorization take?
Our top priority is getting patients insurance coverage, so our partners and affiliated providers do their best to maximize the likelihood of approval.
The prior authorization process usually takes 2-3 weeks but it can be longer if the initial coverage request is denied.
Our partner submits to your insurance company right away. But the process can take longer if more information about your insurance or pharmacy benefits is needed or if there's a secondary plan you want to try.
If your insurance company approves your GLP-1 treatment after that first step, great! If they don't, our partner will continue to work on your behalf. Our partner will see if your insurer requires additional information or will cover a different GLP-1 medication if prescribed.
What happens after I get approved?
Due to several factors, it’s difficult to say precisely when you’ll get medications after prior authorization is approved. One we learn that you’re approved, we’ll send your prescription to your preferred pharmacy and they’ll confirm that there’s medication in stock.
If my prior authorization is approved, when will I get my medication?
Due to several factors, it's difficult to say precisely when you'll get medications after prior authorization is approved. Our partner works with a nationwide network of pharmacies to find the fastest way of getting you started with your medication.
What happens if I get denied?
Our partner will continue to explore all possible options. At this point, your provider will determine whether another GLP-1 medication is clinically appropriate for you. If so, your provider will write a new prescription and the prior authorization process begins again. If all attempts for coverage have been denied and there are no other options, we’ll help you understand cash pay options to see if continued treatment is right for you.
What happens after my insurance approves coverage for the medication?
If you’re prescribed a branded GLP-1 (like Ozempic, Zepbound, or Wegovy) and your coverage is approved, we’ll send your prescription to your preferred pharmacy and they’ll confirm that there’s medication in stock. If your pharmacy doesn’t have supply, they’ll add you to a waitlist for when medication becomes available.
Can you give me the prescription to take to a pharmacy myself?
Unfortunately, no. You can access and download a copy of your prescription in your Ro account, but it’s for reference only and cannot be used to fill or transfer your prescription.
Can I have my prescription sent to my local pharmacy?
Yes, but they may not be able to fill it. You can opt to send your prescription straight to a pharmacy of your choice during your online visit. You can also check with any pharmacy of your choice and let us know if they have your GLP-1 medication in stock. We'll work with our partners to see if it can be filled at that location.
When will I get my medication?
If you’re paying cash, your GLP-1 will ship directly to you in 1-4 days, once prescribed.
If you’re using insurance, it can take 1-2 weeks to receive a decision from your insurance company. Once approved, we’ll send your prescription to your preferred pharmacy for pickup. Your pharmacy should have your prescription ready in 1-2 days, but fulfillment times may vary.
What are savings cards and how can I use them?
Manufacturer savings cards can help reduce the cost of certain branded medications, but eligibility varies.
Savings card details:
Ozempic pen (Novo Nordisk):
If your commercial insurance covers Ozempic, you may be able to pay as low as $25/mo. See eligibility and how to enroll here.
If you’re paying cash for Ozempic, you can pay as low as $499/mo with a manufacturers savings card. See eligibility and how to enroll here.
Wegovy pen (Novo Nordisk):
If your commercial insurance covers the Wegovy pen without a prior authorization, you may save up to $225/mo on your copay. See eligibility and how to enroll here.
If your commercial insurance doesn’t cover it, you can access it by paying cash–either seamlessly delivered to you through Ro’s integration with NovoCare® or with a savings card at your preferred pharmacy.
Cash pay prices through NovoCare® start at $199/mo for the first two months (for a limited time), then $349/mo thereafter. This manufacturer promotional offer is valid through Jun 30. Some restrictions apply.
Zepbound pen (Eli Lilly):
Available through the end of 2026.
If your commercial insurance covers the Zepbound pen, you may save up to $100/mo on your copay.
If your commercial insurance doesn’t cover it, you may save up to $620/mo off the full price.
Note: this savings card program only applies to the Zepbound pen, not the Zepbound single-dose vial. Looking for a simpler, cash-pay option? The Zepbound vial may be a great fit. Learn more here.
Keep in mind:
Savings cards aren’t guaranteed and may vary by pharmacy.
Tell your pharmacist if you’re using a savings card—they may need specific details from it.
Savings cards only apply to branded medications. They can’t be used for compounded GLP-1s through Ro, which are cash-pay only.
If one GLP-1 medication is not covered by my insurance, can I resubmit to my insurance for another medication?
Yes, we do this for you! Ro-affiliated providers survey the clinically appropriate medication options between Wegovy, Ozempic, and Saxenda. If your insurer denies your request for coverage for one of those medications, your provider will see if you’re eligible for the other (if clinically appropriate). Our insurance concierge will resubmit your prior authorization request if you’re eligible.
Can I pay cash for GLP-1 medications?
On Ro, you can access the best available cash-pay prices for FDA-approved GLP-1s like Zepbound KwikPen, Wegovy pen, and Wegovy pill.
Paying the cash pay price could be an option for you if:
GLP-1s are not covered by your insurance
You're uninsured or don’t want to use insurance
Prior authorization is denied, and there are no other coverage options
How much does metabolic testing cost?
If your provider orders a metabolic health test, testing at any Quest location is included in the cost of the Ro Body membership. Or you can purchase an at-home blood collection kit through Ro for $75.
If you live in a state where Quest is not available, we’ll automatically send you an at-home collection kit for no charge.
Can I use government insurance with Ro?
Ro can’t help coordinate coverage for GLP-1 medications for government insurance plans — but depending on your plan, you may still have options to get started.
If you have Medicare, a Medicare supplement plan, or TRICARE: You can join the Ro Body membership and pay out of pocket for certain cash pay medication options. Once you submit a treatment request, a provider will review your info to find the best fit if you’re eligible.
If you have Medicaid or any other government-funded plan: Unfortunately, you can’t join the Ro Body membership or pay out of pocket for treatment through Ro.
If you have a plan through the Federal Employee Health Benefits Program (FEHB): You can join the Ro Body membership and access our insurance concierge. They’ll coordinate your coverage and handle any approval paperwork!