Here's what we'll cover
Here's what we'll cover
Here's what we'll cover

Ro Pharmacy and Ipsos survey finds that physicians and pharmacists believe insurance-centric prescribing rules can negatively impact patients and that extended supply prescriptions, as appropriate, can help improve outcomes among patients on stable, long-term maintenance medications regimens as well as help patients better manage medication costs and adherence.
Physicians and pharmacists partner with patients to help them achieve the best possible health outcomes. This often means helping patients navigate their healthcare journeys including around barriers that can prevent patients from achieving those health outcomes. Those barriers include factors like the cost of a patient’s prescribed treatment, insurance coverage, professional and personal lives, or the availability of local providers or pharmacies.
Ro Pharmacy partnered with Ipsos to survey physicians and pharmacists across the U.S. regarding one potential solution: extended supply prescriptions. Extended supply prescriptions are written and dispensed, when appropriate, to provide patients with 6 to 12 months of supply of their medications. This extended supply is intended to help patients reduce their trips to the pharmacy, save money on refills, and support better adherence to a treatment plan.
Our findings confirm that physicians and pharmacists believe extended supply prescriptions are a patient-centric solution that can help their patients:
navigate access and affordability barriers,
manage their health more effectively,
while reducing the administrative burden on their practice or pharmacy.
WHAT WE EXPLORED
We partnered with Ipsos to survey 400 cardiologists, endocrinologists, primary care practitioners, and pharmacists across the United States about their views of extended supply prescriptions (6 to 12 months of supply).
WHAT WE FOUND
Our survey found that healthcare providers overwhelmingly agree that extended supply prescriptions would not only lead to fewer trips to the pharmacy and reduce the need for less frequent refills, but also improve patient adherence and chronic condition management. In all, 86% of physicians and pharmacists say they would like to be able to write and dispense 6-to-12-month supply prescriptions for their patients on stable regimens of long-term maintenance medications.

Here’s a more detailed breakdown of what surveyed physicians and pharmacists told us:
Adherence: 84% of physicians and pharmacists believe that extended supply prescriptions can help patients on stable regimens of long-term maintenance medications stick with their treatment, ultimately leading to better health outcomes

Convenience: 98% of physicians and 96% of pharmacists believe that extended supply prescriptions would make managing medications more convenient, such as saving patients time by reducing trips to the pharmacy
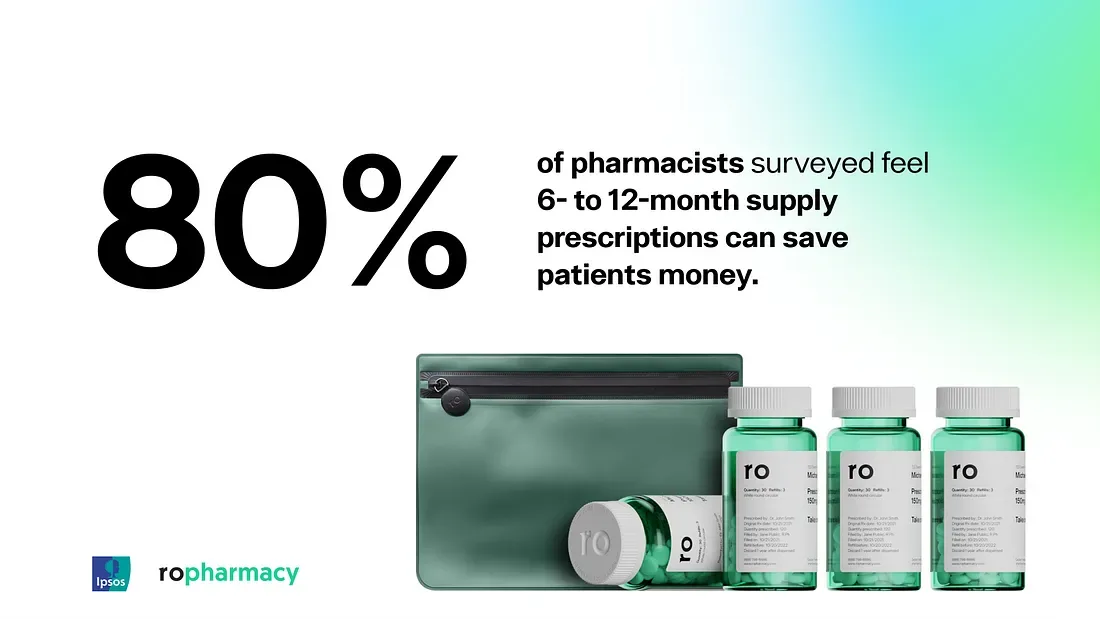
Affordability: 80% of pharmacists believe extended supply prescriptions would save patients money
Safety: 89% of physicians and 73% of pharmacists agree they would feel safe writing and dispensing extended supply prescriptions
Provider Burnout: 91% of physicians agree that extended supply prescriptions could reduce the administrative load for their practice
Providers said that offering extended supply prescriptions would not be without consideration and additional patient education. Surveyed providers highlighted considerations including:
How to dispose of excess medication if a patient needs to titrate their dosage or change medications;
How to refund a patient for unused medication in situations of prescription changes;
How patients could properly store extended supplies of medication;
How to manage extended supply prescriptions and adherence reminders.
THE BIG PICTURE — WHY THIS MATTERS
Offering extended supply prescriptions is one way that direct-to-patient care companies like Ro, via our online pharmacy Ro Pharmacy, are making healthcare more affordable and accessible. For patients, less trips to the pharmacy means savings in time and money — particularly for those living far from their local pharmacy or with one or more chronic conditions, which often require multiple medications and refills.
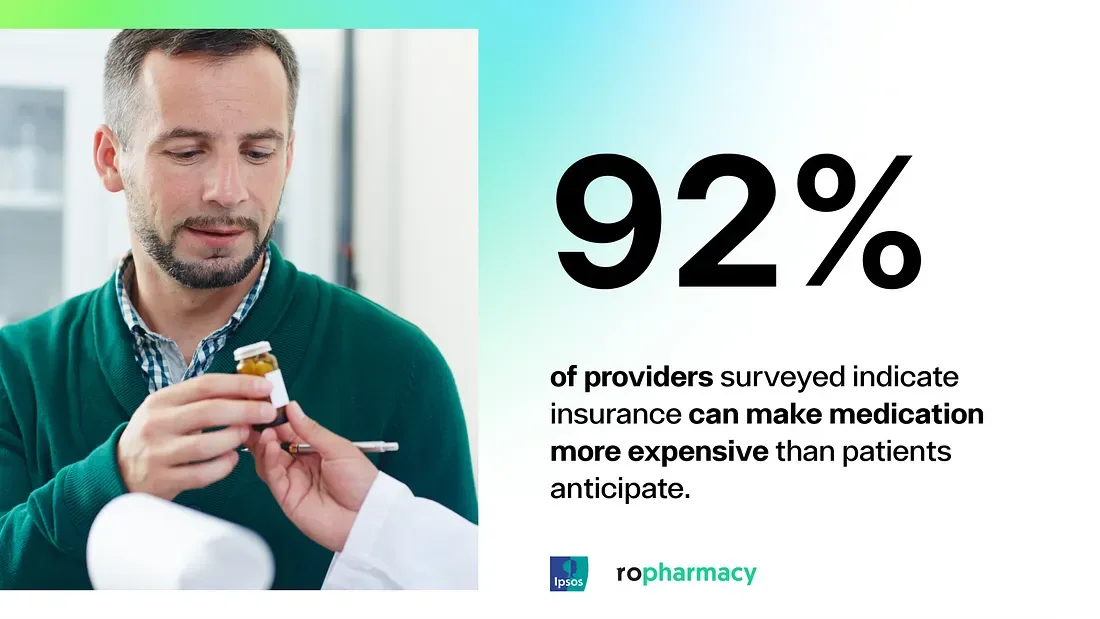
Standard practice today is for providers to prescribe and dispense 30- or 60-day medication supplies. The common practice of limiting drug supplies to 30 to 90 days is largely decided by insurance companies’ rules, not by physicians or pharmacists, and these rules designed to conserve insurance costs and claims. In our survey, providers widely shared that they felt these insurance-centric rules limited their ability to write prescriptions with greater than 30 days of supply between refills (77%), caused them to alter the medication they prescribed (91%), and often made medication more expensive than patients anticipated (92%) when a patient picks up the medication at the pharmacy.
In this system, nearly 30% of American adults report having not taken a prescription as prescribed in the last year due to cost — whether it’s not filling a prescription, skipping or reducing doses, or substituting an over-the-counter medication to save money. And, this behavior — which has been seen at greater rates among lower income households or those with multiple medications — can be quite detrimental to patients’ health.Cost is just one factor that keeps patients from getting the treatments they need. Access and convenience also affect patients. The average wait time at a retail pharmacy is 45 minutes and 1 in 3 neighborhoods in large U.S. cities are pharmacy deserts. Imagine you are a patient managing multiple medications that each require 30-day refills at different dates. Those multiple trips and time — and indirect costs such as time off of work or paying for transportation — can add up and make it even more difficult to keep up with your treatments. Extended supply prescriptions would help patients like this, and many others like them, from those who are immunocompromised, and want to minimize unnecessary risk of exposure, to those who travel often for work, and aren’t necessarily near their local pharmacy.Direct-to-patient healthcare companies, like Ro, use technology to remove barriers, like required insurance coverage, geography, and time constraints, to enable more patients to access the high-quality care and treatments they need. These direct-to-patient models also support physicians and pharmacists by reducing the administrative tasks that contribute to burnout, such as prior authorization, insurance billing, and coding.
“Ro Pharmacy removes the major obstacles to taking medication. Low prices make medicine more affordable and having 6 to 12 months supplies means never running out.”
— Dr. Joycelyn Elders, U.S. Surgeon General (1993–1994) and Ro Medical Advisor
When a patient chooses to fill their prescription, whether from their primary care doctor, specialist, or therapist, through Ro Pharmacy it gives them the option of an extended supply delivered directly to the patient’s doorstep. Our research reinforces that physicians and pharmacists agree that these extended supply prescriptions, available in our direct-to-patient pharmacy, can be affordable, safe, and help patients to better manage their medications and health.
ABOUT THE STUDY
These are the findings from an Ipsos poll conducted from May 24 to June 4, 2021 on behalf of Ro Pharmacy. For the survey, a sample of 400 cardiologists, endocrinologists, primary care practitioners, and pharmacists from the continental U.S., Alaska and Hawaii was interviewed online in English.To qualify, cardiologists, endocrinologists, and primary care practitioners must have initiated prescription medication regimens for their patients and have patients currently prescribed a stable maintenance medication regimen.Statistical margins of error are not applicable to online non-probability polls. All sample surveys and polls may be subject to other sources of error, including, but not limited to coverage error and measurement error. Where figures do not sum to 100, this is due to the effects of rounding. The precision of Ipsos online polls is measured using a credibility interval. In this case, the poll has a credibility interval of plus or minus 5.6 percentage points for all respondents. Ipsos calculates a design effect (DEFF) for each study based on the variation of the weights, following the formula of Kish (1965). This study had a credibility interval adjusted for the design effect of the following (n=400, DEFF=1.5, adjusted Confidence Interval = +/-7.1 percentage points for all respondents).