Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
We updated our analysis in February of 2021 using 2020 government data on primary care deserts and our most recent patient data. Between our original and updated analysis, the number of primary care deserts grew from 1722 to 1884. Meanwhile, Ro increased its reach into rural deserts (going from 84% coverage to 95% coverage), and now serves patients in 98% of urban deserts.
There are simply not enough physicians to meet our nation’s growing health care needs. Here at Ro, our goal is for our direct-to-consumer (DTC) telemedicine platform to bridge these access gaps, and we hold ourselves accountable by using research and data to evaluate our progress. To find out whether patients in underserved communities are adopting telemedicine as a solution, we conducted an analysis to determine whether we are in fact providing treatment in parts of the country where access to care is a challenge.
Turns out, we are already serving patients in many of the communities that do not have enough primary care physicians to meet local needs — a sign that telemedicine can increase access and reduce health disparities for patients regardless of where they live.
The demand for physicians is far outpacing supply
According to a report released this summer by the Association of American Medical Colleges (AAMC), the United States will see a shortage of up to nearly 139,000 physicians, across all specialty and practice types by 2032. Of this shortage, nearly half — 55,200 — are expected to be primary care physicians. These latest projections are indeed alarming, but for many Americans, the long wait times and long travel times required to see a provider is a current reality.
Already, physicians aren’t geographically distributed in direct proportion to the population, creating a mismatch between supply and demand in many communities. Telemedicine offers a solution by allowing patients to access a wider network of doctors, preventing geography from being a limiting factor to access to care, and ensuring Americans get the care they need regardless of where they choose to live.
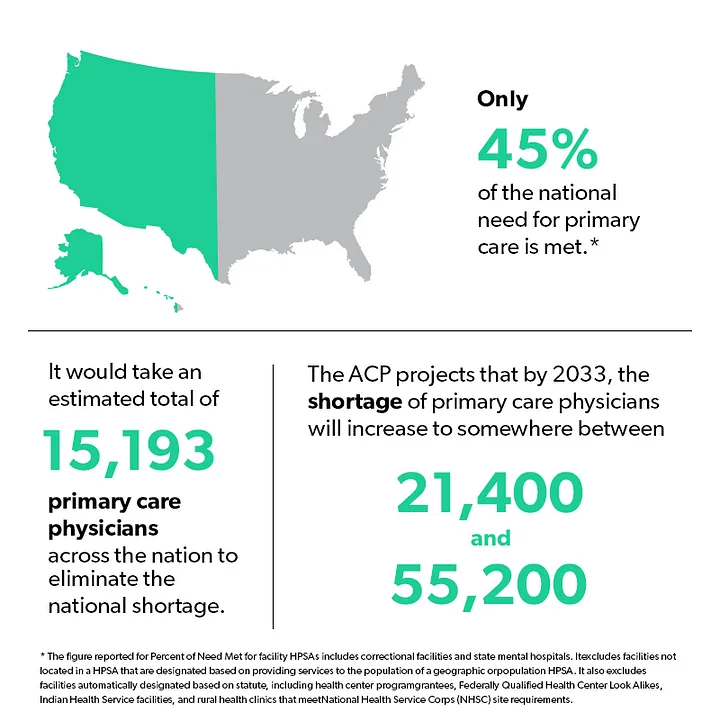
Source: https://www.aamc.org/news-insights/press-releases/new-aamc-report-confirms-growing-physician-shortage and https://data.hrsa.gov/Default/GenerateHPSAQuarterlyReport
We analyzed our internal data to find out if telemedicine is bridging the access gap for underserved patients residing in Primary Care Deserts. It is.
At Ro, we strive to make it easier for all Americans to receive high-quality health care when they need it, but especially for those who are currently struggling with access barriers. We wanted to know whether we are indeed bridging the care gap in areas where access is a challenge: specifically, in areas already experiencing primary care physician shortages.
What is a ‘Primary Care Desert’?
To start, we categorized communities that do not have enough primary care physicians to support local needs as Primary Care Deserts.
To do this, we applied the classification system used by the Health Resources & Services Administration (HRSA) branch of the federal government that identifies certain geographies in the United States as having an official shortage of practicing primary care professionals. The federal government refers to these areas as Primary Care Health Provider Shortage Areas, or Primary Care HPSAs. Under this system, counties in the United States can fall into one of three categories:
the whole county is designated as a Primary Care HPSA, i.e. across the entire county, there are not enough primary care physicians to meet the local need
part of the county is designated as a Primary Care HPSA, i.e. some parts of the county do not have enough primary care physicians to meet local needs, but other parts of the county are not experiencing any kind of shortage
none of the county is designated as a Primary Care HPSA, i.e. there are enough primary care physicians distributed across the entire county to meet the local need
We determined a Primary Care Desert to be any county that is classified as an entire-county HPSA, because these are the areas that are experiencing the most widespread shortage issues.
Once we classified which counties are Primary Care Deserts, we wanted to know how many patients being treated on Ro’s platform actually live in one, and therefore might be using DTC telemedicine to fill an access gap created by the lack of primary care physicians in their community. We geolocated our members within their county of residence, and then cross-checked that list against our list of Primary Care Deserts.
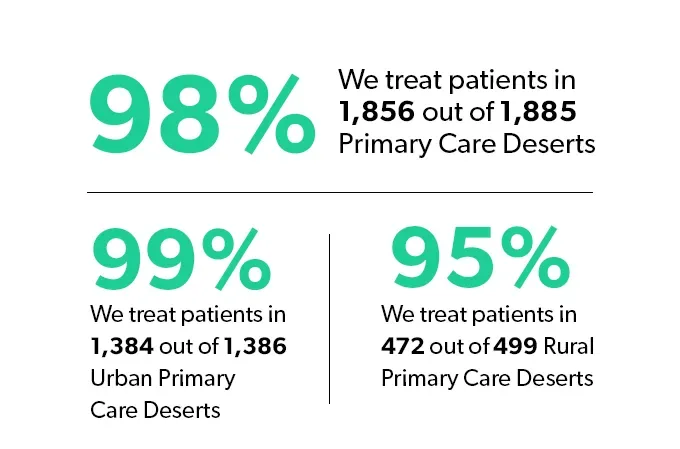
We found that Ro is bridging the gap: of the 1,884 Primary Care Deserts, we treat patients in 1868 of them — 98%.
Urban and Rural Communities
One key feature of Primary Care Deserts is that they include both urban and rural communities. It is well known that health disparities, especially around access, exist across the urban/rural divide (a topic that I have researched extensively in the past: read more about it here and here), and the challenges of receiving health care in a Primary Care Desert are likely very different depending on which kind of community someone resides in.
We further broke down our analysis across urban and rural Primary Care Deserts to identify whether Ro’s platform is increasing access in the most remote and isolated communities.
To distinguish between urban and rural primary care deserts, we used the U.S. Department of Agriculture’s Rural Urban Commuting Codes (RUCC) system. RUCC codes split counties into either metro or non-metro, and then further distinguish urbanity/rurality within those categories. The table below describes their 9 point classifier:
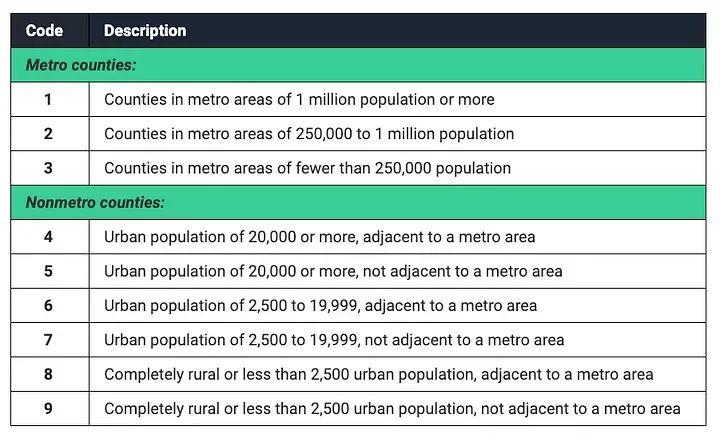
Source: RUCC Codes
We split Primary Care Deserts into urban and rural by lumping counties with RUCC codes 1-7 into the urban category, and RUCC codes 8 and 9 into the rural category.We created a map depicting which counties are considered Primary Care Deserts, distinguishing between counties classified as deserts that exist in either rural or urban communities using the above clusters of RUCC codes.
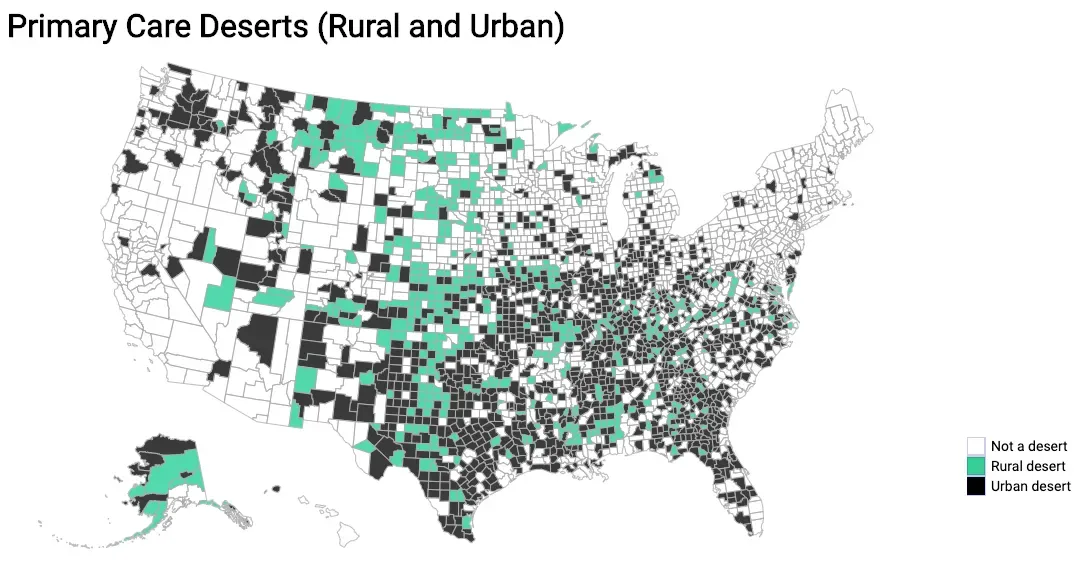
Our map is interactive! Click here to learn more about each Primary Care Desert.
According to our data, Ro treats patients in almost 100% of urban Primary Care Deserts (1384 out of 1385), but more importantly, we treat patients in 95% of rural Primary Care Deserts (472 out of 499).
Our findings indicate that as DTC telemedicine improves access, it is not leaving rural communities behind. Instead, we are making strides to reduce urban/rural health disparities by improving access to care for everyone.
We know that telemedicine can’t solve every problem associated with primary care provider shortages: some conditions require in-person care, and we believe it is important for patients to have a primary care physician with whom they have an ongoing relationship. But for the many conditions that can be treated virtually as a supplement to in-person primary care, telemedicine can meaningfully improve people’s health, and their lives, no matter how far they live from a provider.