Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
Everyone is familiar with acne, and most people have experienced it at some point in their lives. However, cystic acne is more than just a few inconvenient zits. It is a more severe type of acne that can be distressing and even painful. But don’t despair! Treatment options can help clear your skin and improve your self-esteem.
Read on to learn more about cystic acne and how to get rid of it.
What is cystic acne?
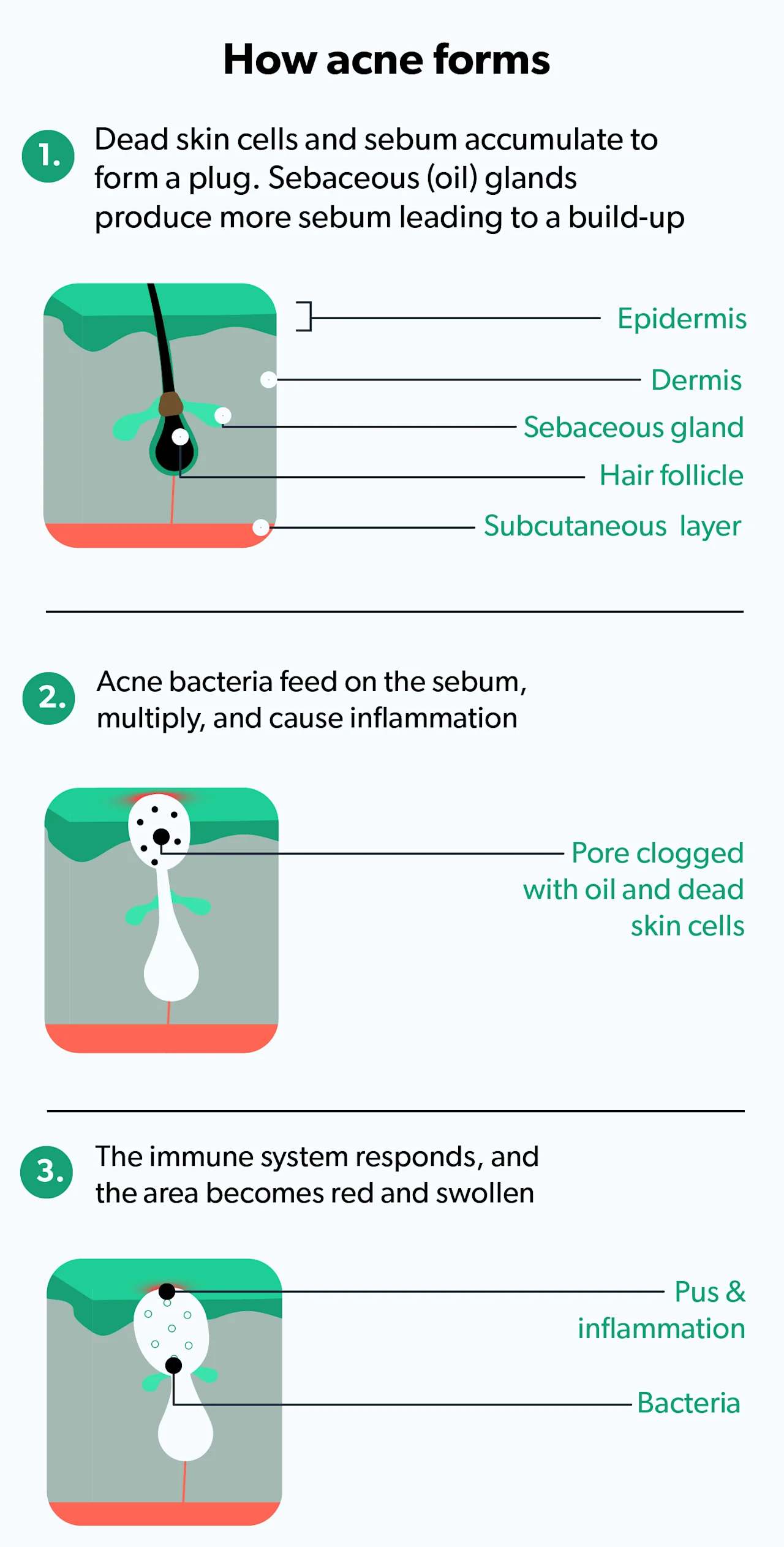
To understand how cystic acne forms, you first need to understand how acne forms. Acne (also known as acne vulgaris) occurs when a skin pore, or sebaceous (oil-producing) follicle, becomes clogged with excess oil (sebum) and dead skin cells.
These clogged pores can become inflamed or infected with skin bacteria (Oge', 2019). Cystic acne (also known as nodular acne) forms when the inflammation goes deep into the skin.
Signs and symptoms of cystic acne
Cystic acne is more severe than typical acne breakouts. Common signs and symptoms include (Oge’, 2019):
Large, solid, bumps beneath the skin
Large, pus-filled lumps (pustules) beneath the skin
Redness (erythema)
Pain or tenderness
Scars or dark spots on skin from past breakouts that have healed
Risk factors and causes of cystic acne
Cystic acne is caused by many of the same things that trigger less severe forms of acne. Several factors can lead to "breakouts," including (Oge’, 2019):
Genetics
Hormonal changes, like during your menstrual cycle
Lifestyle factors, like diet and cigarette smoking
Medical issues like polycystic ovary syndrome (PCOS)
Medications like corticosteroids
How to treat cystic acne
Severe acne, like cystic acne, often needs to be treated with oral prescription medications because over-the-counter products are not strong enough.
These pills are systemic medications that have effects throughout the body (as opposed to topical drugs that you apply directly to the site of your acne). The treatments include retinoids like isotretinoin, oral antibiotics, oral birth control pills, and antiandrogen agents like spironolactone.
Isotretinoin
Isotretinoin (brand name Accutane) is a retinoid (a drug that comes from vitamin A) that is very effective in treating the underlying causes of severe acne (Zouboulis, 2015).
Isotretinoin stops your sebaceous glands from producing too much oil—this decreases skin bacteria growth and reduces its ability to cause infection and inflammation. All of these effects boil down to improvements in your cystic acne (Fallah, 2021).
Here are some key things to take note of regarding using isotretinoin:
The typical treatment usually lasts for at least 4–6 months, but some people need longer courses of the medication. After starting this treatment, you may notice an initial flare-up of inflammation within the first 3–4 weeks. This gets better on its own over time (Pile, 2021).
You must avoid getting pregnant before or during treatment because isotretinoin has a high risk of harming a developing fetus. To start this therapy, you must be willing to have regular pregnancy tests. You should also use two forms of contraception while you’re taking isotretinoin (Pile, 2021).
Less serious side effects you may experience with isotretinoin include dryness of your skin, eyes, mouth, and nose. It also makes your skin more sensitive to the sun and prone to sunburns (photosensitivity). Make sure to wear sunscreen daily while on this treatment (Pile, 2021).
Oral antibiotics
Oral antibiotics are an effective cystic acne treatment because of their antibacterial effect and their ability to decrease inflammation (anti-inflammatory effect). Tetracycline antibiotics, including doxycycline and minocycline, are the most common oral antibiotics for cystic acne (Oge’, 2019).
When taking oral antibiotics for the treatment of cystic acne, some things to keep in mind are (Zaenglein, 2016):
Side effects of these drugs include increased photosensitivity, upset stomach, diarrhea, and skin discoloration.
Pregnant people and children under eight years old should not use tetracyclines.
In general, you should limit the amount of time you are on oral antibiotics (no more than 3–4 months) to prevent antibiotic resistance.
Antibiotics are often combined with other treatments (like benzoyl peroxide or retinoids) to further decrease the risk of antibiotic resistance (Zouboulis, 2015).
Other systemic antibiotic options include erythromycin and azithromycin. However, these are usually reserved for people who cannot take tetracyclines, like pregnant people or children under eight years of age (Zaenglein, 2016).
Oral birth control pills
Birth control pills can restore the balance of estrogens and other hormones in women, leading to clearer skin.
Combined oral contraceptives (CACs), which are birth control pills with both estrogens and progestins, are the most effective at treating acne. Birth control pills can help decrease the androgen (male hormone) levels in the skin, which leads to reduced oil production and improved acne. Four combined oral contraceptives are currently FDA-approved for treating acne in women (Zaenglein, 2018):
Estrogen and norgestimate (brand name Ortho Tri-Cyclen)
Estrogen and norethindrone (brand name Estrostep)
Estrogen and drospirenone (brand name Yaz)
Estrogen and drospirenone and levomefolate (brand name Beyaz)
It can take several months for your acne to improve on oral birth control pills, so some dermatologists recommend combining CACs with other treatments, like retinoids (Oge', 2019).
Common side effects include weight gain, breast tenderness, and breakthrough bleeding. Rarely, more serious adverse effects like blood clots and heart attacks may occur in some women, especially women over 35 years of age. Oral birth control pills are not recommended for women over 35 (Cooper, 2021).
Spironolactone
Like oral birth control pills, spironolactone affects your hormone balance and blocks androgens in the skin. It can trigger breast development in men, so spironolactone is usually only given to women.
With this treatment, you may begin to see a decrease in breakouts and skin oiliness within a few weeks. Some people experience side effects like painful or irregular periods, breast tenderness, and breast enlargement. Spironolactone is not recommended for pregnant women (Zaenglein, 2018).
Steroid injections
Some people with cystic acne may benefit from injecting a steroid medication directly into the cysts or nodules to help quickly reduce size and pain. Improvement can occur relatively rapidly with these injections. Side effects include thinning skin in the area of the injection (Zaenglein, 2016; Oge’, 2019).
Cystic acne and acne scarring
Cystic acne can cause permanent scarring as it heals, more often than less severe types of acne.
Atrophic scars are the most common types of scarring that people experience after their acne breakouts clear up. Atrophic scars are due to the loss of collagen at the acne site, resulting in depressions (holes or pits) in the skin. The three most common atrophic scarring shapes are (Boen, 2019):
Ice pick scars: narrow, deep holes
Boxcar scars: round to oval holes with vertical edges
Rolling scars: wider pits give a rolling appearance to the skin
Less commonly, you can form hypertrophic scars; these are raised, pink, firm scars that occur more frequently on the trunk and in darker-skinned people (Ogawa, 2017).
How to treat acne scarring
Ideally, the best way to treat acne scars is to be proactive and prevent them from forming in the first place. You can accomplish this by seeking treatment for your acne early. Avoid picking or popping your acne cysts, which increases the risk of infection and scarring. Try to wash your face each evening, and after sweating, with a gentle cleanser—never scrub your face. You should also wear sunscreen anytime you are in the sun.
Despite all of these measures, some people still end up with acne scars. Fortunately, several treatments can help but may require more than one session to achieve optimal results.
Chemical peels: Chemical peels use harsh chemicals to remove the outer layers of skin and allow new skin and collagen to grow. They typically use solutions of salicylic acid, glycolic acid, pyruvic acid, or trichloroacetic acid (TCA) (Boen, 2019).
Dermabrasion: Dermabrasion uses a device with an abrasive material to remove the outer layers of skin, triggering the wound healing process and forming new collagen (Boen, 2019).
Laser therapy: Laser treatments use light of varying strengths and wavelengths to affect different parts of the skin. Two types of laser therapies are available to treat acne scars: ablative and non-ablative. Ablative lasers (carbon dioxide and erbium YAG lasers) remove the outer layers of skin, while non-ablative lasers (Nd:YAG and diode lasers) target the deeper tissue without affecting the overlying skin (Boen, 2019).
Skin needling: Skin needling uses a small roller with tiny needles to create multiple punctures in the superficial layers of skin. The skin develops micro bruises that stimulate healing and new collagen formation (Boen, 2019).
How to prevent cystic acne
No solution can completely prevent cystic acne. Think about the causes of cystic acne: some can change (like your skincare routine), while others cannot (like your genetics). By addressing the risk factors you can control, you may make acne less likely to develop. The less acne you have, the less likely you are to have cystic acne.
Some things you can do to try to prevent cystic acne are:
Check your skin and hair products to make sure that they say things like non-comedogenic, oil-free, non-acnegenic, or “won’t clog pores.”
Adopt a healthy skincare regimen. Wash your face with a gentle cleanser and pat it dry every morning and evening and after sweating. Use moisturizers regularly to avoid allowing your skin to become too dry.
Try using alcohol-free cosmetics (and makeup removers) that are less likely to dry out your skin.
Always remove your makeup before bedtime
Do not pop your acne pimples
When to see a dermatologist
If you are suffering from cystic acne, consult a dermatologist, and start treatment early. This can improve not only your skin health and potential scarring but also other symptoms like depression, anxiety, and low self-esteem.
While you may feel embarrassed by your blemishes, they can be treated. It may take some time, but by working with your dermatologist, you can find the therapy that works best for you.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
References
American Academy of Dermatology (AAD). (n.d.). Skin conditions by the numbers . Retrieved November 2, 2021 from https://www.aad.org/media/stats-numbers
Boen, M., & Jacob, C. (2019). A review and update of treatment options using the acne scar classification system. Dermatologic Surgery: Official Publication for American Society for Dermatologic Surgery , 45 (3), 411–422. doi: 10.1097/DSS.0000000000001765. Retrieved from https://pubmed.ncbi.nlm.nih.gov/30856634/
Cooper, D. B., & Mahdy, H. (2021). Oral contraceptive pills. [Updated Aug 25, 2021]. In: StatPearls [Internet]. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK430882/
Fallah, H., & Rademaker, M. (2021). Isotretinoin in the management of acne vulgaris: practical prescribing. International Journal of Dermatology, 60 (4), 451–460. doi: 10.1111/ijd.15089. Retrieved from https://pubmed.ncbi.nlm.nih.gov/32860434/
Ogawa, R. (2017). Keloid and hypertrophic scars are the result of chronic inflammation in the reticular dermis. International Journal of Molecular Sciences , 18 (3), 606. doi: 10.3390/ijms18030606. Retrieved from https://pubmed.ncbi.nlm.nih.gov/28287424/
Oge', L. K., Broussard, A., & Marshall, M. D. (2019). Acne vulgaris: diagnosis and treatment. American Family Physician , 100 (8), 475–484. Retrieved from https://pubmed.ncbi.nlm.nih.gov/31613567/
Pile, H. D., Sadiq, N. M. (2021). Isotretinoin. [Updated May 10, 2021]. In: StatPearls [Internet]. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK525949/
Zaenglein, A., Pathy, A., Schlosser, B., Alikhan, A., Baldwin, H., & Berson, D. et al. (2016). Guidelines of care for the management of acne vulgaris. Journal Of The American Academy Of Dermatology , 74 (5), 945-973.e33. doi: 10.1016/j.jaad.2015.12.037. Retrieved from https://pubmed.ncbi.nlm.nih.gov/26897386/
Zaenglein, A. L. (2018). Acne vulgaris. The New England Journal of Medicine , 379 (14), 1343–1352. doi: 10.1056/NEJMcp1702493. Retrieved from https://pubmed.ncbi.nlm.nih.gov/30281982/
Zouboulis, C., & Bettoli, V. (2015). Management of severe acne. British Journal Of Dermatology , 172 , 27-36. doi: 10.1111/bjd.13639. Retrieved from https://pubmed.ncbi.nlm.nih.gov/25597508/






