Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
It’s easier said than done, but if you have erectile dysfunction, try not to stress about it and get help from a healthcare professional instead. Stress and anxiety are among many potential underlying causes or contributing factors to ED. And in a double downer, cause-and-effect can be a two-way street: The frustration of erectile dysfunction can induce stress, anxiety, depression, and other mental health issues.
Luckily, there are effective treatments for both ED and mental health conditions. Let’s learn more about the relationship between these conditions.
ED is common and treatable
Erectile dysfunction affects a man’s ability to get and maintain an erection long enough for satisfactory sexual intercourse (Velurajah, 2021). The condition is widespread: the percentage of men who struggle with firmness rises with age, being less than 10 percent of men under 50, about 20–40 percent after age 60, then above 50 percent after age 70 (Maiorino, 2015).
Many studies have shown that stress, anxiety, depression, and other mental health conditions can contribute to erectile dysfunction. Fortunately, these conditions are often treatable—either with self-care strategies and lifestyle changes or through professional therapy or medications. The first step is for you and your healthcare provider to determine what is causing what.
Mental health and ED: a vicious cycle
The primary underlying cause of ED in men over 50 is atherosclerosis, an issue with the cardiovascular system which provides blood flow to all body parts, including the penis. Atherosclerosis, a hardening and narrowing of the arteries, can thwart the flow of blood to your penis, where it’s needed when all goes well. But mental health conditions like stress and anxiety can also cause or contribute to ED, directly and indirectly.
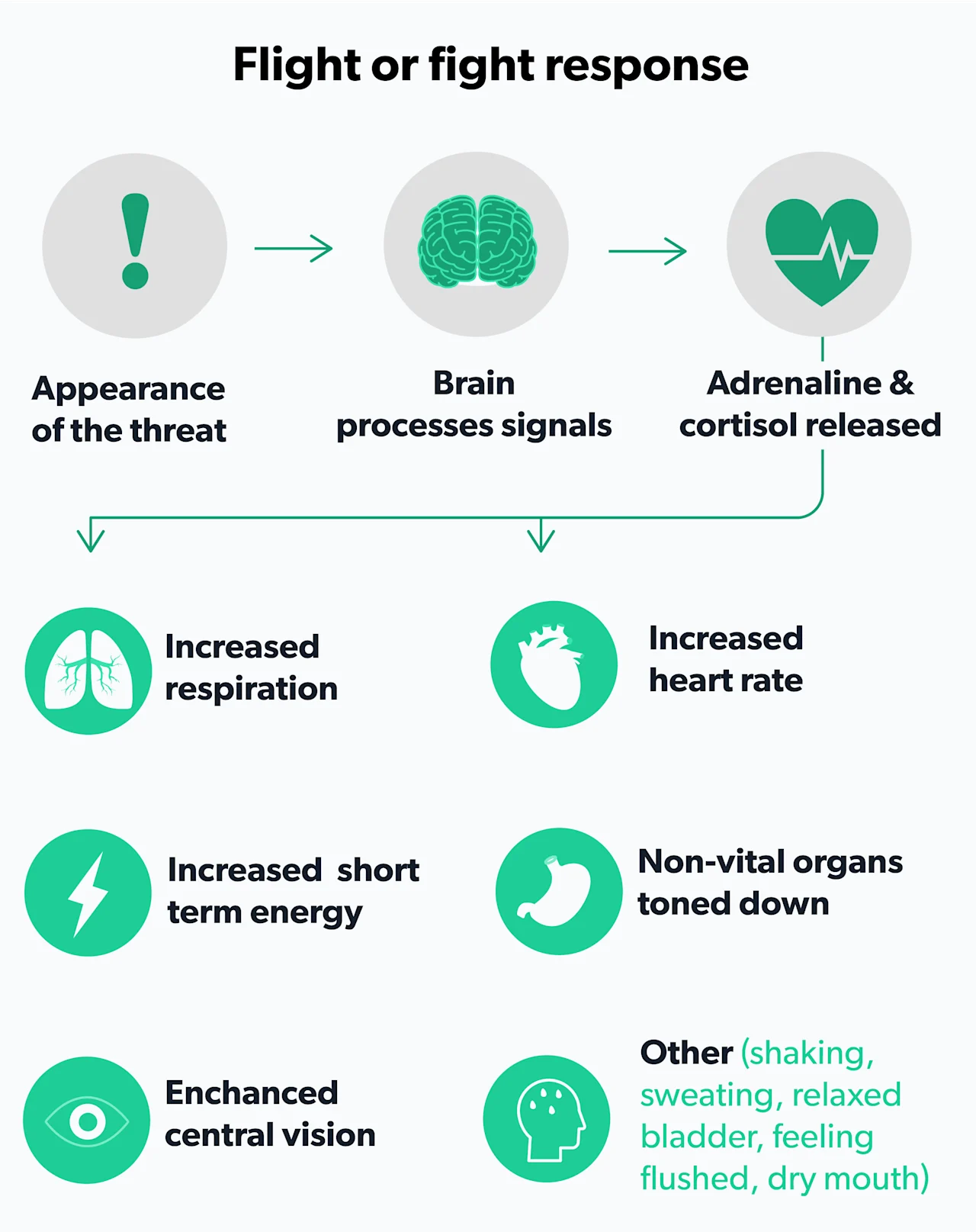
Stress causes the body to release a hormone called cortisol, which in the short run, is vital to our fight-or-flight responses. But when stress is chronic, the release of cortisol over time can cause inflammation throughout the body (Hannibal, 2014). Such chronic stress and cortisol release can also impede the production of testosterone, which in turn can then lead to ED (Rivas, 2014).
Chronic stress contributes to atherosclerosis, the hardening of the arteries that restricts that all-important blood flow (Yao, 2019). Anxiety, too, has been shown to lead to poor cardiovascular health, again a risk factor for ED (Celano, 2016).
One small study found that among men with ED, premature ejaculation, and other sexual dysfunctions, 12.5 percent also had diagnosable depression, and 23.4 percent had anxiety disorders. Those mental disorders are often undiagnosed, the researchers found (Rajkumar, 2015). A separate review of all research on the topic found that some 37 percent of men with ED also have one of these anxiety disorders: post-traumatic stress disorder, obsessive-compulsive disorder, social phobia/social anxiety disorder, or panic disorder (Velurajah, 2021).
Which is causing which?
It seems it can go either way. According to a broad review of studies, ED can fuel lower self-esteem and low sexual satisfaction, causing stress and making a man more susceptible to anxiety and depression. While the relationship between mental health and ED is not fully understood, it’s thought they can interact negatively back-and-forth (Velurajah, 2021).
How a man and his partner respond to ED “can lead to a vicious cycle of increased uneasiness, distance, and conflicts. This, in turn, leads to a lower frequency of sexual encounters, less time spent together and lack of communication between partners in a relationship” (Hedon, 2003).
How to treat ED
Several lifestyle changes have been shown to boost moods and help people relax, and which can help alleviate ED problems directly by improving blood flow to your penis (Maiorino, 2015):
Increase your level of physical activity.
Eat more vegetables and fruits, whole grains, and legumes.
Avoid smoking and excess alcohol.
The value of exercise can’t be overstated, specifically for lessening ED and more generally for increasing and improving sexual activity. Men who are physically more active have more sex and fewer problems with erectile dysfunction (Smith, 2019).
If stress, anxiety, or depression are getting in the way of your sex life and you’re unable to fix them with lifestyle changes, it may be time to seek help from a healthcare professional. Likewise, you’ll want to make sure there isn’t some other serious health problem behind your flaccidity, such as high blood pressure, diabetes, or a sleep disorder.
Treatments that are often helpful for stress, anxiety, and depression include:
Mindfulness and mindfulness meditation: teaching you to be in the moment, more relaxed, aware, and accepting of the pleasures and challenges in life.
Cognitive-behavioral therapy (CBT): guided sessions that force the recognition of negative thoughts and teach coping skills.
Antidepressants and other medication: typically prescribed in addition to lifestyle changes and talk therapies, or when those other options don’t work (Bandelow, 2017). Among the unfortunate possible side effects of many antidepressants and anti-anxiety medications, however: erectile dysfunction. (Higgins, 2010).
If you’re struggling with erectile dysfunction and lifestyle changes don’t remedy the problem, it’s time to seek help from a healthcare provider. They may recommend medication or other treatments. Your healthcare provider can help you find the best treatment or combination of remedies to get you back in the game.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
References
Bandelow B, Michaelis S, Wedekind D. (2017). Treatment of anxiety disorders. Dialogues in Clinical Neuroscience; 19 (2):93-107. doi: 10.31887/DCNS.2017.19.2/bbandelow. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5573566/
Celano CM, Daunis DJ, Lokko HN, Campbell KA, Huffman JC. (2016). Anxiety disorders and cardiovascular disease. Current Psychiatry Report; 18 (11):101. doi: 10.1007/s11920-016-0739-5. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5149447/
Hannibal KE, Bishop MD. (2014). Chronic stress, cortisol dysfunction, and pain: a psychoneuroendocrine rationale for stress management in pain rehabilitation. Physical Therapy; 94 (12):1816-1825. doi: 10.2522/ptj.20130597. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4263906/
Hedon, F. (2003). Anxiety and erectile dysfunction: a global approach to ED enhances results and quality of life. International Journal of Impotence Research 15 , S16–S19. doi: 10.1038/sj.ijir.3900994. Retrieved from https://www.nature.com/articles/3900994
Higgins A, Nash M, Lynch AM. (2010). Antidepressant-associated sexual dysfunction: impact, effects, and treatment. Drug, Healthcare, and Patient Satisfaction; 2 :141-150. doi: 10.2147/DHPS.S7634. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3108697/
Martin SA, Atlantis E, Lange K, Taylor AW, O'Loughlin P, Wittert GA, et al. (2014). Predictors of sexual dysfunction incidence and remission in men. Journal of Sexual Medicine; 11 (5):1136-47. doi: 10.1111/jsm.12483. Retrieved from https://onlinelibrary.wiley.com/doi/abs/10.1111/jsm.12483
Maiorino MI, Bellastella G, Esposito K. (2015). Lifestyle modifications and erectile dysfunction: what can be expected?. Asian Journal of Andrology; 17 (1):5-10. doi: 10.4103/1008-682X.137687. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4291878/
Mayo Clinic. (2021). Erectile dysfunction. Retrieved from https://www.mayoclinic.org/diseases-conditions/erectile-dysfunction/symptoms-causes/syc-20355776
Rajkumar RP, Kumaran AK. (2015). Depression and anxiety in men with sexual dysfunction: a retrospective study. Comprehensive Psychiatry; 60 :114-8. doi: 10.1016/j.comppsych.2015.03.001. Retrieved from https://pubmed.ncbi.nlm.nih.gov/25818906/
Rivas AM, Mulkey Z, Lado-Abeal J, Yarbrough S. (2014). Diagnosing and managing low serum testosterone. Proctology (Baylor University Medical Center); 27 (4):321-324. doi: 10.1080/08998280.2014.11929145. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4255853/
Smith L, Grabovac I, Yang L, Veronese N, Koyanagi A, Jackson SE. (2019). Participation in physical activity is associated with sexual activity in older English adults. International Journal of Environmental Research and Public Health; 16 (3):489. doi: 10.3390/ijerph16030489. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6388286/
Velurajah, R., Brunckhorst, O., Waqar, M. et al. (2021). Erectile dysfunction in patients with anxiety disorders: a systematic review. International Journal of Impotence Research (2021). doi: 10.1038/s41443-020-00405-4. Retrieved from https://www.nature.com/articles/s41443-020-00405-4
Yao BC, Meng LB, Hao ML, Zhang YM, Gong T, Guo ZG. (2019). Chronic stress: a critical risk factor for atherosclerosis. Journal of International Medical Research; 47 (4):1429-1440. doi: 10.1177/0300060519826820. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6460614/










