Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
High blood pressure can be a pain. It can cause headaches, but frequently it has no symptoms at all. You might even find out that you have high blood pressure entirely by chance during a routine check at your yearly physical. But even when there are no symptoms involved, it can really limit how you live your life. While there are a lot of medications out there to treat high blood pressure, they don’t all work the same way.
Your healthcare provider will likely select the best treatment option for you and make adjustments based on how you respond. So if you’ve recently started lisinopril or losartan, or if your healthcare provider decided to switch you from one to the other, you might be wondering what the difference is. Here’s what you need to know about each of these medications, how they differ, and why your healthcare provider may choose one for you instead of the other.
While both lisinopril and losartan can be used to treat high blood pressure, they each do more than that. Lisinopril, part of a class of medications called ACE-inhibitors, is approved by the FDA as part of the treatment for heart failure, which is a condition that occurs when the heart has trouble effectively pumping blood around the body (DailyMed, 2019). Losartan, part of a class of medications known as ARBs (angiotensin receptor blockers), has been shown to reduce the risk of having a stroke (blood clot in the brain) and reduce damage to the kidneys in people who have diabetes.
So while both drugs treat high blood pressure, your healthcare provider might select a particular medication based on your personal medical history. Also, each drug has a different set of side effects. The most common side effects of ACE inhibitors like lisinopril include a persistent, dry cough. Some people find this bothersome enough to switch medications, in which case your healthcare provider may switch you to an ARB like losartan (Mann, 2020).
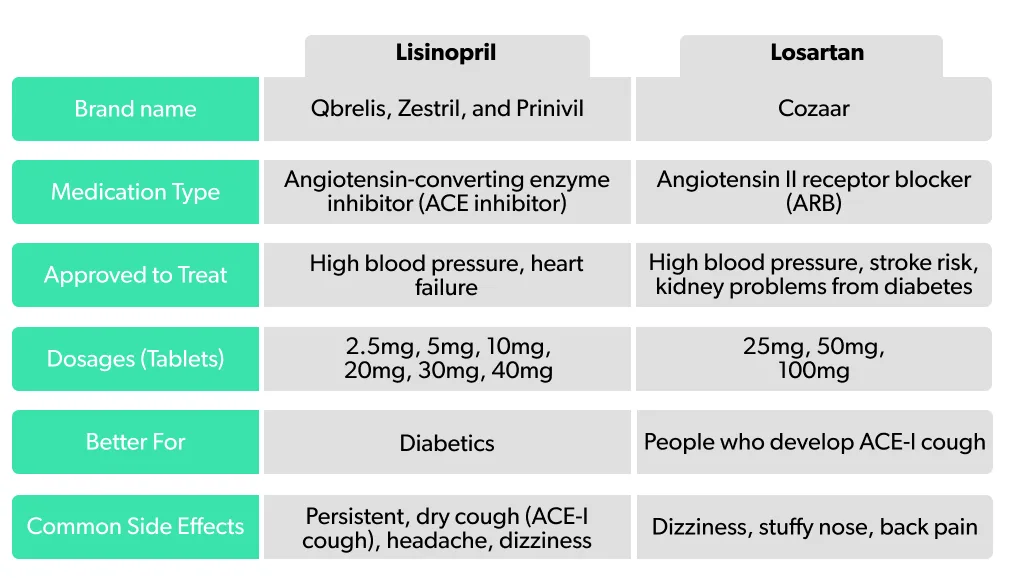
Lisinopril is the generic name for a prescription medication commonly sold under the brand names Qbrelis, Zestril, and Prinivil. It belongs to a class of medications called angiotensin-converting enzyme inhibitors (ACE inhibitors) (DailyMed, 2019).
Lisinopril is approved by the U.S. Food and Drug Administration (FDA) to treat high blood pressure (hypertension) (FDA, 2016). Losartan potassium is the generic name for the prescription drug commonly sold under the brand name Cozaar. Like lisinopril, it’s approved by the FDA to treat high blood pressure, but it belongs to a different class of medications called angiotensin II receptor blockers (ARBs) (DailyMed, 2020).
Though both of these prescription medicines may be used to lower blood pressure and prescribed with other medications, they're not prescribed together because there may be serious side effects. Like ARBs, ACE inhibitors such as lisinopril act on the renin-angiotensin-aldosterone system (RAAS). When combined with ARBs such as losartan, these medications may increase your risk of low blood pressure (hypotension), high potassium levels (hyperkalemia), fainting (syncope), and worsening kidney function. It may even cause kidney failure (DailyMed, 2020).
Although ARBs and ACE inhibitors are related and act on the same system in order to lower blood pressure, they interfere with different parts of the system. Angiotensin II is a hormone that's part of your RAAS, and it causes blood vessels to constrict (get smaller).
Think of a four-lane highway suddenly merging to become a one-lane highway - there's going to be a lot of traffic and pressure there). Too much angiotensin may lead to high blood pressure over time. This hormone also affects the amount of antidiuretic hormone (ADH) that's released by the body, which also contributes to maintaining blood pressure.
ARBs block the actions of angiotensin II, whereas ACE inhibitors block an enzyme that makes angiotensin II (Burnier, 2001; Sweitzer, 2003). These prescription drugs relax the blood vessels resulting in lower blood pressure (DailyMed, 2020). Since these medications work in different ways, one may be more effective than the other for some people, and their side effects may differ.
General guidelines state that either ACE-inhibitors or ARBs can be prescribed as first-line treatment for high blood pressure. Your healthcare provider may choose based on the differences mentioned below. If you're started on an ACE-inhibitor and develop the dry, persistent cough associated with this medication, you may be switched to an ARB.
Which is better in which situation?
Some people simply do not tolerate ACE inhibitors, and they'll develop side effects that other people may not. For example, if you have type 2 diabetes and high blood pressure, your healthcare provider may prescribe lisinopril. One study directly compared the effects of losartan and lisinopril in non-diabetic patients with hypertension. Researchers found that lisinopril improved insulin sensitivity in patients, whereas losartan did not. This was the biggest difference between the treatments. The medications improved blood pressure roughly the same amount, giving neither one an edge in treating high blood pressure (Fogari, 1998). But the effect on insulin sensitivity may give lisinopril a slight advantage in treating hypertensive patients who also have diabetes.
The best treatment for you may not be one of these medications alone, however—especially if you're at a higher risk of cardiac events. Both ACE inhibitors and ARBs may be combined with either thiazide diuretics (drugs that encourage water loss in the form of urine, reducing blood volume) or dihydropyridine calcium-channel blockers (antihypertensive drugs), and some organizations such as the European Society of Cardiology (ESC) and the European Society of Hypertension (ESH) recommend starting with combination therapy for people with severe hypertension (Williams, 2018).
One study that looked at over 11,000 patients with hypertension found that an ACE inhibitor combined with a calcium-channel blocker was more effective at reducing cardiac events such as non-fatal heart attack and stroke than an ACE inhibitor combined with thiazide diuretics (Jamerson, 2008).
What is losartan?
Losartan belongs to a drug class called angiotensin receptor blockers (ARBs) that also includes valsartan and irbesartan. This prescription medication is approved by the U.S. Food and Drug Administration (FDA) to treat high blood pressure (hypertension), stroke risk, and kidney problems from diabetes (DailyMed, 2020).
However, it may not be as effective at reducing stroke risk in Black people with high blood pressure and left ventricular hypertrophy (enlarged heart) (DailyMed, 2020). It may also be used off-label after a heart attack to help individuals with heart failure who cannot tolerate ACE inhibitors and treat non-diabetic kidney disease (UpToDate, n.d.).
Losartan is available both as generic losartan potassium tablets and as brand name Cozaar. Tablets are available in 25 mg, 50 mg, and 100 mg strengths. In people with high blood pressure, the most common side effects of losartan include upper respiratory infection, dizziness, stuffy nose, and back pain. In individuals with type 2 diabetes taking losartan to manage kidney problems, the most common side effects are chest pain, diarrhea, high blood potassium, low blood pressure, low blood sugar, and tiredness (FDA, 2018).
Serious side effects are possible with losartan and may include severe allergic reaction—including hives, itching, rash, and trouble breathing—low blood pressure (hypotension), high blood potassium (hyperkalemia), and changes in kidney function that may include kidney failure in some cases (UpToDate, n.d.). Hyperkalemia can be mild or serious, potentially causing heart problems such as arrhythmias (irregular heartbeat), muscle weakness, or paralysis (Simon, 2020).
Losartan may also cause serious adverse effects when combined with certain medications, such as lithium, non-steroidal anti-inflammatory drugs (NSAIDs), ACE inhibitors, and aliskiren, a renin inhibitor that's also used to lower blood pressure (DailyMed, 2020). You should stop taking losartan if you become pregnant as the drug may cause fetal death or injury if taken during the second or third trimester (final six months of pregnancy) (FDA, 2018). Tell your healthcare provider or pharmacist about what other drugs or supplements you're taking before starting so they can advise on your specific case.
What is lisinopril?
Lisinopril belongs to the class of medications called angiotensin-converting enzyme (ACE) inhibitors along with medications such as ramipril, captopril, and enalapril. ACE-I medications are all antihypertensive drugs, meaning they're approved by the U.S. Food and Drug Administration (FDA) to treat high blood pressure (hypertension) (DailyMed, 2019; FDA, 2016). It may also be used as an additional therapy for individuals with heart failure and for the treatment of heart attack (acute myocardial infarction) (FDA, 2016).
In those with high blood pressure, the most common side effects are headache, dizziness, and cough. Those taking lisinopril for heart failure may experience low blood pressure (hypotension)—which may cause fainting (syncope) and dizziness—and chest pain. The most common adverse effect in those taking this medication after a heart attack is low blood pressure.
Lisinopril may also cause kidney problems or high blood potassium levels (hyperkalemia). If rapid swelling (angioedema) happens—including swelling of the face, lips, tongue, and extremities—this may be a sign of an allergic reaction. If this happens, stop taking lisinopril immediately and get medical attention right away (FDA, 2016).
There are also potential drug interactions when taking lisinopril. Like losartan, lisinopril may cause adverse effects when mixed with non-steroidal anti-inflammatory drugs (NSAIDs) and lithium. It also should not be mixed with diuretics or other medications such as ARBs that act on the renin-angiotensin system as this may increase your risk of dangerously low blood pressure. Combining lisinopril with ARBs may also increase your risk of kidney problems and high blood potassium (FDA, 2016).
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
References
Burnier, M. (2001). Angiotensin II Type 1 Receptor Blockers. Circulation, 103 (6), 904-912. doi:10.1161/01.cir.103.6.904. Retrieved from https://www.ahajournals.org/doi/10.1161/01.cir.103.6.904
DailyMed. (2019). PRINIVIL- lisinopril tablet. Retrieved from https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=f6f3c339-2c9d-4d07-14a1-6d6c7daf26c6
DailyMed. (2020). Losartan Potassium tablets 25 mg, film coated. Retrieved from https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=a3f034a4-c65b-4f53-9f2e-fef80c260b84
Fogari, R., Zoppi, A., Corradi, L., Lazzari, P., Mugellini, A., & Lusardi, P. (1998). Comparative effects of lisinopril and losartan on insulin sensitivity in the treatment of non diabetic hypertensive patients. British Journal of Clinical Pharmacology, 46 (5), 467-471. doi:10.1046/j.1365-2125.1998.00811.x. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1873694/
Food and Drug Administration (FDA). (2016, October). PRINIVIL (lisinopril) tablets label. Retrieved from https://www.accessdata.fda.gov/drugsatfda_docs/label/2016/019558s060lbl.pdf
Food and Drug Administration (FDA). (2018, October). Cozaar (losartan potassium) label. Retrieved from https://www.accessdata.fda.gov/drugsatfda_docs/label/2018/020386s062lbl.pdf
Jamerson, K., Weber, M. A., Bakris, G. L., Dahlöf, B., Pitt, B., Shi, V., et al. (2008). Benazepril plus Amlodipine or Hydrochlorothiazide for Hypertension in High-Risk Patients. New England Journal of Medicine, 359 (23), 2417-2428. doi:10.1056/nejmoa0806182. Retrieved from https://www.nejm.org/doi/10.1056/NEJMoa0806182
Mann, J. (2020, October). Choice of drug therapy in primary (essential) hypertension. UptoDate. Retrieved Nov. 3, 2020 from https://www.uptodate.com/contents/choice-of-drug-therapy-in-primary-essential-hypertension
Simon, L. V., Hashmi, M. F., & Farrell, M. W. (2020). Hyperkalemia . In: StatPearls. Treasure Island, FL: StatPearls Publishing. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK470284/
Sweitzer, N. K. (2003). What Is an Angiotensin Converting Enzyme Inhibitor? Circulation, 108 (3), E16-E18. doi:10.1161/01.cir.0000075957.16003.07. Retrieved from https://www.ahajournals.org/doi/full/10.1161/01.cir.0000075957.16003.07
UpToDate. (n.d.). Losartan: Drug Information. Retrieved from https://www.uptodate.com/contents/losartan-drug-information?search=losartan&source=panel_search_result&selectedTitle=1~69&usage_type=panel&kp_tab=drug_general&display_rank=1#F25472738
Williams, B., Mancia, G., Spiering, W., Rosei, E. A., Azizi, M., Burnier, M., et al. (2018). 2018 ESC/ESH Guidelines for the management of arterial hypertension. European Heart Journal, 39 (33), 3021-3104. doi:10.1093/eurheartj/ehy339. Retrieved from https://academic.oup.com/eurheartj/article/39/33/3021/5079119



