Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
One in ten women has polycystic ovary syndrome, or PCOS (yep — it’s that prevalent), but it often goes undiagnosed. Below, we’re digging into what you need to know about PCOS and how a simple hormone test can help you and your doctor find out if you have it.
What is PCOS?
Polycystic ovary syndrome, or PCOS, is a hormone imbalance that often results in irregular periods and cycles without ovulation. Common symptoms of PCOS can include weight gain, insulin resistance, oily skin and/or acne, thinning hair on the scalp, and excessive unwanted hair growth, typically in places like the face, chest, and back.

Most of the time, PCOS is undiagnosed — but it’s very common.
Is there a test for PCOS diagnosis?
The test for PCOS is actually a bunch of different tests. Doctors use something called the Rotterdam criteria (it’s basically a checklist) to diagnose PCOS. These criteria include:
Irregular or absent menstrual cycles
High levels of male sex hormones like testosterone or symptoms that might indicate high levels (like acne or excessive hair growth)
An increased number of immature follicles in the ovaries
If a doctor is able to check at least two out of the three boxes and rule out any other potential causes of your symptoms, you’ll be diagnosed with PCOS.

PCOS diagnosis relies on the Rotterdam criteria.
How does a hormone test help inform a PCOS diagnosis?
Modern Fertility tests up to seven hormones — one of which can help your doctor decide if you need additional evaluation for PCOS.
While AMH (anti-Mullerian hormone) isn’t part of the Rotterdam criteria, it can also be helpful when it comes to determining if someone might have PCOS. Why? High AMH may indicate that the ovaries contain large numbers of immature follicles. (Reminder: A high number of immature follicles is third on the checklist for PCOS.) When it comes to diagnosing PCOS, though, that third criterion is evaluated using an ultrasound examination.
The cells that surround immature follicles produce AMH. The more immature follicles, the more AMH. Science backs this up: Women with PCOS have higher levels of AMH on average when compared to women who don’t have the condition.
That brings us to the “cyst” in polycystic. The cysts are the immature follicles in the ovaries. When there’s a higher number of these immature follicles (polycystic), you can see them using an ultrasound.
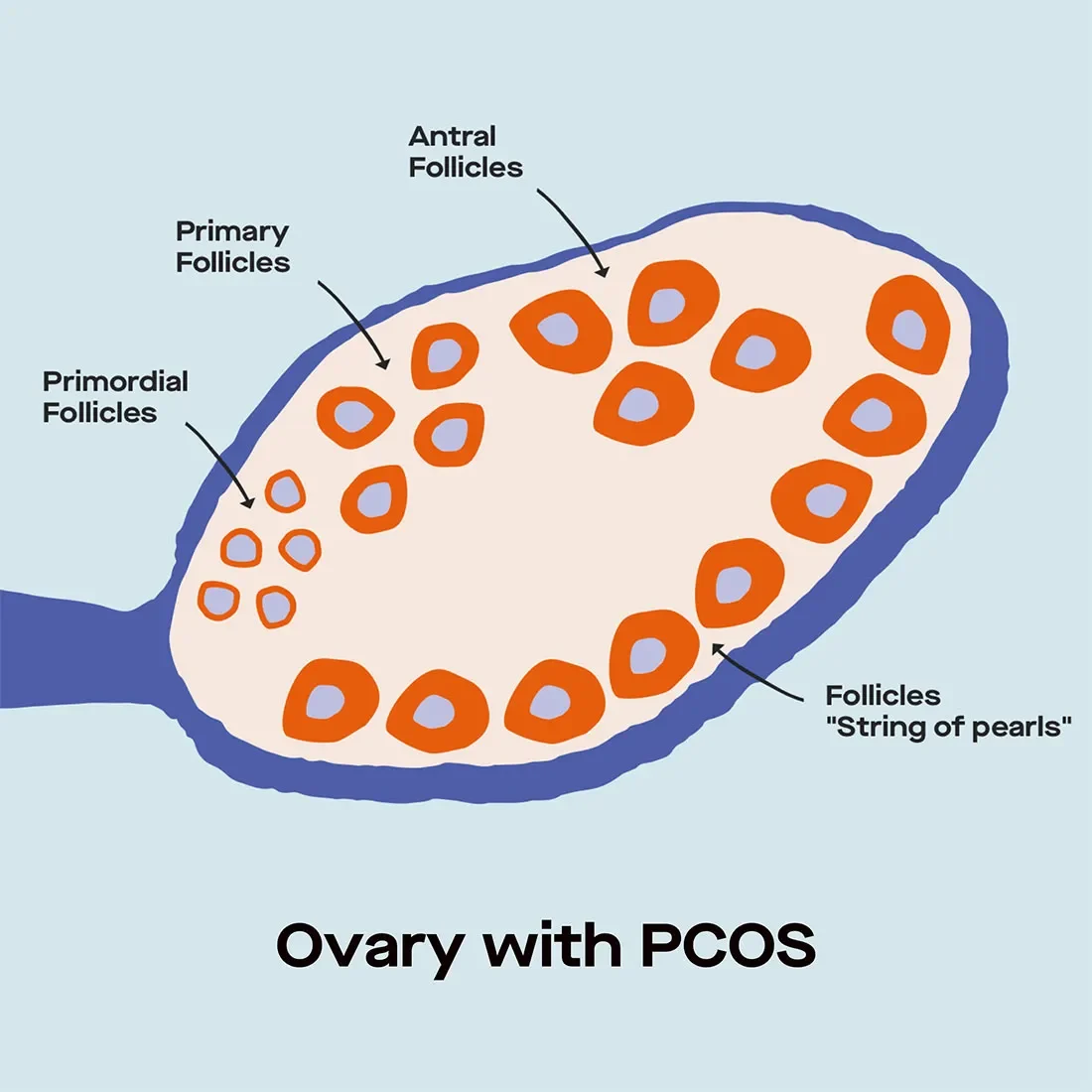
PCOS causes “string of pearls” follicles in the ovaries.
How do you get a formal PCOS diagnosis?
Only a healthcare provider can diagnose PCOS. But if you read the Rotterdam criteria and think that two out of three apply to you, here’s what you can expect if you bring a possible PCOS diagnosis up with your doctor.
Your provider will likely ask about how regular your cycle is — and potentially follow up with another blood test to check your testosterone levels, as well as the levels of other hormones in order to rule out other potential causes of your symptoms.
In some cases, your doctor will suggest a transvaginal ultrasound to take a look at your ovaries.
How might PCOS affect fertility?
The biggest barrier to getting pregnant with PCOS is ovulation. Because PCOS often means that lots and lots of eggs start developing each month in the ovaries but many cycles are actually anovulatory (i.e. no egg is released) there often isn’t an egg to fertilize. That’s why infertility is so common among people with PCOS.
But treatment for PCOS can often help with ovulation too. For people with PCOS who have overweight, weight management can help restore ovulatory function. Also, there are a few different medications (such as clomiphene and letrozole) that can help too.
If those methods don’t end up regulating ovulation, in-vitro fertilization (IVF) can also help women with PCOS get pregnant. The bottom line is that there are lots of options — and a doctor can help you plan the best strategy for you.
PCOS can affect ovulation and make getting pregnant more difficult.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.









