Women's Health Articles
Many health concerns are universal—heart disease, diabetes, skin cancer—but women have many unique health needs. From birth control and pregnancy to endometriosis and PCOS, there’s a wide range of issues unique to those with female anatomy. Please note: We know (and celebrate!) that not everyone who identifies as a woman has a vagina, ovaries, or a uterus (and vice versa). If you cannot find what you are looking for in this category, please explore our other health categories as well.
8 MIN READ
Can Ozempic help with PCOS?
7 MIN READ
PCOS (polycystic ovarian syndrome)
4 MIN READ
Does Ozempic interfere with birth control?
5 MIN READ
Is Ozempic safe while pregnant?
4 MIN READ
Low testosterone in women
4 MIN READ
High testosterone in women
4 MIN READ
Do you gain weight on your period?
3 MIN READ
Where is the clitoris located?
6 MIN READ
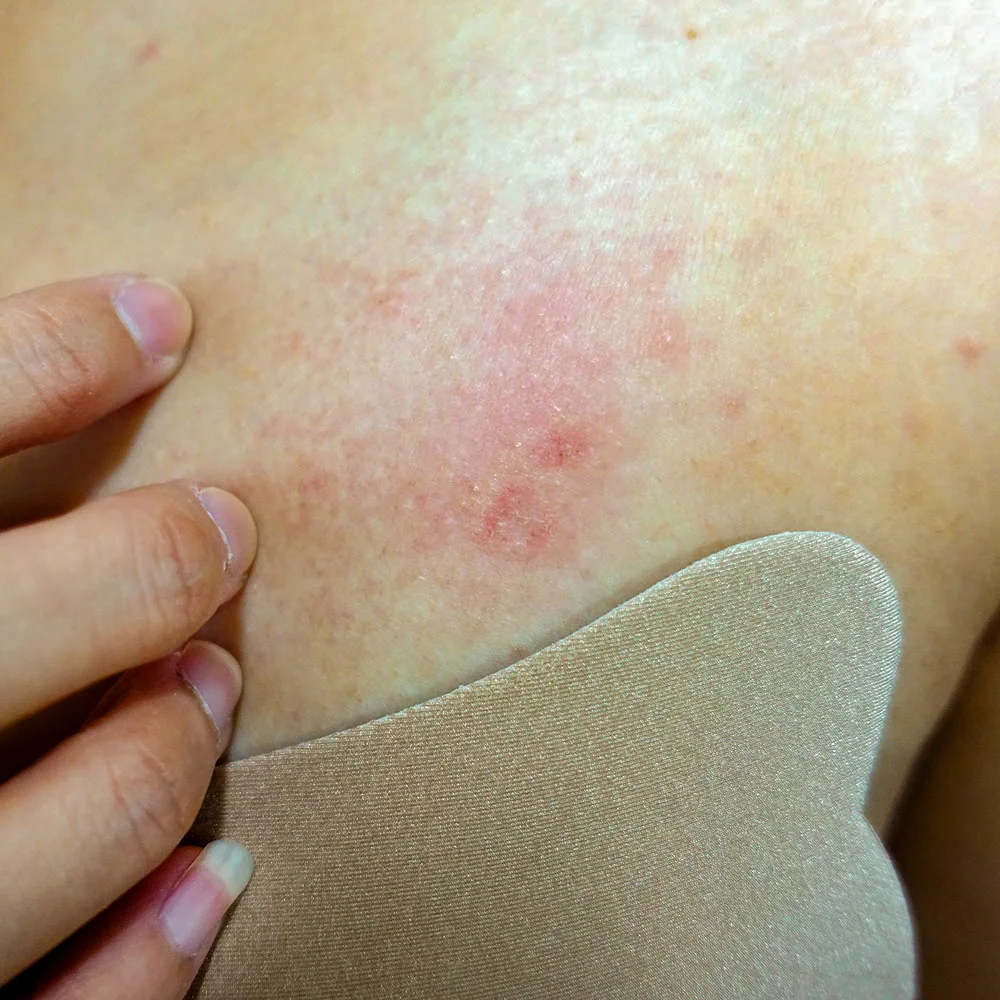
Rash on breast
4 MIN READ
Signs and symptoms of breast cancer
5 MIN READ
Paget's Disease of the Breast
4 MIN READ
Bacterial vaginosis OTC treatment