Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
Each year, breast cancer makes up around 10% of all new cancer diagnoses. Breast cancer predominantly affects females and is the second leading cause of death in women worldwide (Alkabban, 2021).
Understanding the signs and symptoms, especially some of the less common ones, might be one of the best ways to ensure early detection and treatment, increasing survival rates. Annual breast cancer screening using mammograms can reduce the chance of dying from breast cancer by roughly 40% (Monticciolo, 2021).
While self-examination can be nerve-wracking, it’s good to keep in mind that even if you do find something abnormal, most lumps and breast tissue changes are actually benign (not cancer). Around 3-6% of changes evaluated by healthcare providers are associated with underlying cancer (Stachs, 2019).
Still, it’s important to get checked as soon as you find something out of the ordinary. If it is a sign of something more serious, the earlier you find it and get treatment the better the outcome.
Signs and symptoms of breast cancer
The first warning signs often start with breast changes. A lump is the most frequent symptom of breast cancer, presenting as the main complaint in 83% of new cases. Around 1 in 6 people diagnosed with breast cancer show other symptoms, such as breast pain and changes to the nipple or surrounding skin (Koo, 2017).
How breast cancer appears can differ significantly from person to person, but the most common signs include (Parthasarathy, 2012; Koo, 2017):
A new lump or mass in the breast or armpit
Swollen or painful lymph nodes in the armpit, collarbone, or underarm area
Swelling or thickening in any part of the breast
Dimpling or puckering of breast skin (known by healthcare providers as peau d'orange, which means orange skin in French)
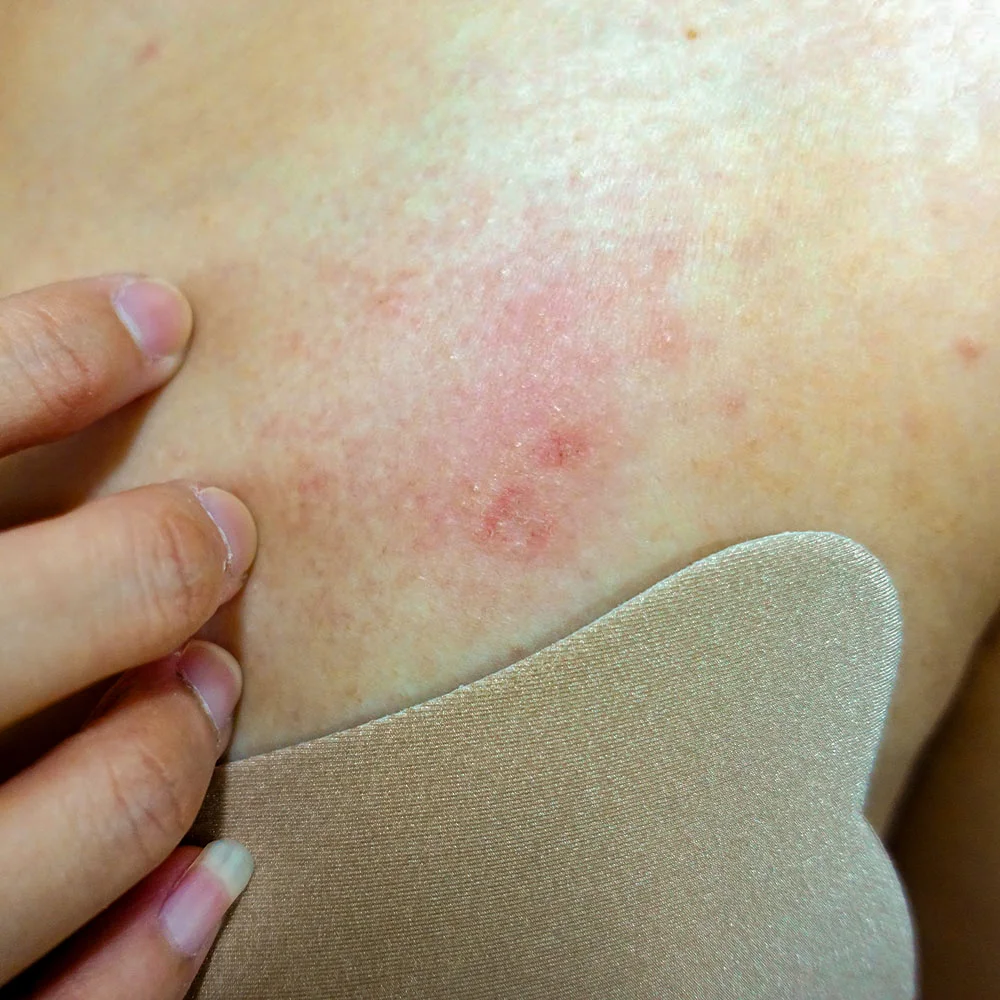
Redness, flaking, scaliness, itchiness, or irritation in the breast, nipple, or areola
Inversion or flattening of the nipple
Nipple or breast pain
Nipple discharge that’s not breast milk in a person who is lactating (blood, pus, or whitish discharge)
New sudden changes in the size, shape, or appearance of one or both breasts
Any other change in how your breasts feel that’s not explained by being pregnant or breastfeeding, your menstrual cycle, menopause, recent weight gain or loss, or a side effect of medication
Some symptoms are more common to certain types of breast cancer. For example, inflammatory breast cancer is often accompanied by inflammation that causes swelling or redness. The rarer Paget’s disease is associated with changes to the nipple area that are sometimes described as looking like eczema (Alkabban, 2021).
Only you know how your breasts feel––that’s why you’re most likely to be the first to notice any changes. Breasts are just as individual as people and what’s “normal” can vary. Keep an eye out for these symptoms and any other irregularities related to your breasts. If you notice any, speak to a gynecologist or healthcare provider.
How to detect early signs of breast cancer
Over half of all breast cancers are discovered through a clinical breast exam or a patient reporting something they found to their doctor (Roth, 2011).
To find potential signs as soon as possible, schedule breast cancer screenings regularly each year. This includes a physical breast exam and (typically starting at age 40) annual mammograms (Monticciolo, 2021).
How to do a breast self-exam
At home, you can perform your own monthly breast exams. A study found that 1 in 4 people with breast cancer found it themselves while doing their own exam (Roth, 2011).
It’s best to do it around the same time each month, usually after your period (if you menstruate), since breast changes are normal during the hormonal fluctuations associated with menstruation. Here’s what to do (Pippin, 2021):
While undressed, stand facing the mirror with your shoulders straight and arms by your sides. Turn to the right so that your left profile is facing the mirror, and then turn to the right. Do your breasts and nipples look their usual size, shape, and color?
Next, raise your arms over your head and bend forward. Perform the same visual exam from all three angles (facing the mirror and from both your left and right profiles). Does everything look normal? There should be no discharge, skin texture or color changes, or new bulging, or changes in shape.
Stand up once more. Place your hands on your hips and hunch forward. Look at your breasts from all three angles and confirm that nothing looks unusual.
Now, lie down and examine each breast with the opposite hand. Using the pads of your index and middle fingers, firmly touch your entire breast in small increments. You can go in circular patterns or up and down, as long as you investigate every part all the way from your armpits to your collarbone. Keep your fingers in constant contact with the skin to avoid skipping over any breast tissue. Do you feel any lumps or changes in skin texture around your nipples or breasts?
When to see a doctor
If you have any concerns or notice changes in your breasts, schedule an appointment with a healthcare provider for further evaluation.
Remember, some of the above symptoms can be caused by other skin or breast conditions that are not cancerous. Examples are eczema, fibrocystic breast disease, and cysts. While these are benign, it’s a good idea to see a healthcare provider to make sure and get proper treatment if necessary.
In the meantime, stay consistent with annual breast cancer screenings. Mammograms can detect tumors in the early stages before any physical symptoms of breast cancer develop (Monticciolo, 2021).
If you have an increased risk of breast cancer based on your family history or if the BRCA1 or BRCA2 genes run in your family, ask a healthcare provider what steps you can take to ensure early detection and lower your risk.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
References
Alkabban, F. M., & Ferguson, T. (2021). Breast Cancer. In StatPearls. StatPearls Publishing. Retrieved from https://pubmed.ncbi.nlm.nih.gov/29493913/
Koo, M. M., von Wagner, C., Abel, G. A., McPhail, S., Rubin, G. P., & Lyratzopoulos, G. (2017). Typical and atypical presenting symptoms of breast cancer and their associations with diagnostic intervals: Evidence from a national audit of cancer diagnosis. Cancer Epidemiology, 48, 140–146. doi: 10.1016/j.canep.2017.04.010. Retrieved from https://pubmed.ncbi.nlm.nih.gov/28549339/
Monticciolo, D. L., Malak, S. F., Friedewald, S. M., Eby, P. R., Newell, M. S., Moy, L., et al. (2021). Breast cancer screening recommendations inclusive of all women at average risk: Update from the ACR and Society of Breast Imaging. Journal of the American College of Radiology, 18 (9), 1280–1288. doi: 10.1016/j.jacr.2021.04.021. Retrieved from https://pubmed.ncbi.nlm.nih.gov/28648873/
Parthasarathy, V., & Rathnam, U. (2012). Nipple discharge: an early warning sign of breast cancer. International Journal of Preventive Medicine, 3 (11), 810–814. Retrieved from https://pubmed.ncbi.nlm.nih.gov/23189234/
Pippin, M. M., & Boyd, R. (2021). Breast Self Examination. In StatPearls. StatPearls Publishing. Retrieved from https://pubmed.ncbi.nlm.nih.gov/33351405/
Roth, M. Y., Elmore, J. G., Yi-Frazier, J. P., Reisch, L. M., Oster, N. V., & Miglioretti, D. L. (2011). Self-detection remains a key method of breast cancer detection for U.S. women. Journal of Women's Health, 20 (8), 1135–1139. doi: 10.1089/jwh.2010.2493. Retrieved from https://pubmed.ncbi.nlm.nih.gov/21675875/
Stachs, A., Stubert, J., Reimer, T., & Hartmann, S. (2019). Benign breast disease in women. Deutsches Arzteblatt International, 116 (33-34), 565–574. doi: 10.3238/arztebl.2019.0565. Retrieved from https://pubmed.ncbi.nlm.nih.gov/31554551/