Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
We like to think of periods as the fifth vital sign alongside body temperature, blood pressure, pulse (heart rate), and breathing rate. Many of us may think that tracking our period and ovulation is exclusively for understanding when we’re most fertile in hopes of getting pregnant.
But learning more about your ovulation patterns, menstrual cycle, and overall fertility can help you in a lot of ways that have nothing to do with trying to conceive. Here are four good reasons why you should still track your ovulation — even if you’re not trying to conceive.
1. To understand your body's hormonal patterns after coming off birth control.

When many of us first start navigating our birth control options, we may be frustrated by the lack of accurate information available to us. Articles about birth control usage may include fear-mongering language and any potential side effects and impact to fertility can be confusing — making an intimate medical decision even more overwhelming.
Uterus owners often must teach themselves about their own reproductive systems because, historically, that kind of healthcare is not prioritized by the medical community. If you're hoping to gather more information about your body’s general functions and to demystify your reproductive system, tracking your cycle and ovulation is a great place to start.
Ovulation tests can be an especially useful tool if you are transitioning off of hormonal birth control and want to relearn your body’s patterns. Hormonal birth control (like the pill) works to prevent ovulation using estrogen and/or progestin (sometimes a combo of the two). Keep in mind that progestin-only birth control doesn’t consistently stop ovulation — about 40% of women who use progestin-only pills will continue to ovulate. (In those cases, birth control works in other ways to effectively prevent pregnancy, if that's your goal.)
“I’ve been on some sort of birth control since I was 16 years old. I am 34 now,” says Cindy H., a member of our Modern Community. Now that she is ending hormonal birth control use for the first time in almost two decades, she's started tracking her cycle. “I plan on learning a little more about my body, and just seeing what my body normally does without the influence of exogenous hormones,” (the kinds of hormones found in oral contraceptives and hormonal IUDs and implants).
Each individual may experience different side effects of hormonal birth control. When you track ovulation and periods after stopping hormonal birth control, you can document unfamiliar aspects of your cycle so you can better manage your period moving forward.
2. To easily anticipate your period, and connect the dots between your cycle and unexplained symptoms.

As Chair of the Modern Fertility Medical Advisory Board Dr. Nataki Douglas, MD, says, “Understanding your cycle and predicting your period are linked.”
Have you ever been surprised by the arrival of your period, finding yourself without any menstrual hygiene products left at home or in your bag? (That’s a situation many of us know all too well.) Or maybe you get killer cramps and rely on certain medications to ease your pain, and you forgot to head to the pharmacy because you didn’t realize you’d be needing relief so soon.Tracking your cycle is a great way to anticipate your period: It helps you learn the usual lengths of your periods, the regularity (or irregularity) of your cycle, and its likely start date that month. That way, you’re as prepared as possible to care for your symptoms and flow as soon as they happen.
Dr. Eva Luo, OB-GYN, says tracking your cycle in order to anticipate your period is particularly helpful when your periods are heavy and/or painful since you may need even greater pain relief or more access to menstrual hygiene products. Dr. Luo has personally experienced dysmenorrhea, which is a term used to describe especially painful periods. Dr. Luo says, “If I saw that my period was about to start and I did not have ibuprofen on hand, I knew it was time to make that purchase.“Endometriosis, an often painful health condition where tissue similar to the uterine lining grows outside of the uterus, can also contribute to especially painful periods. Dr. Luo says people with endometriosis can similarly use cycle tracking to aid with their pain management during menstruation, too.But tracking your cycle can help you understand and prepare for symptoms of discomfort beyond your period and menstrual pain. Depending on where you are in your cycle, you can experience different symptoms including vaginal discharge changes, breast tenderness, bloating, and general abdominal discomfort. But if you’ve never tracked your cycle, you might never recognize these issues as related.
3. To track other health issues (like thyroid conditions or PCOS).
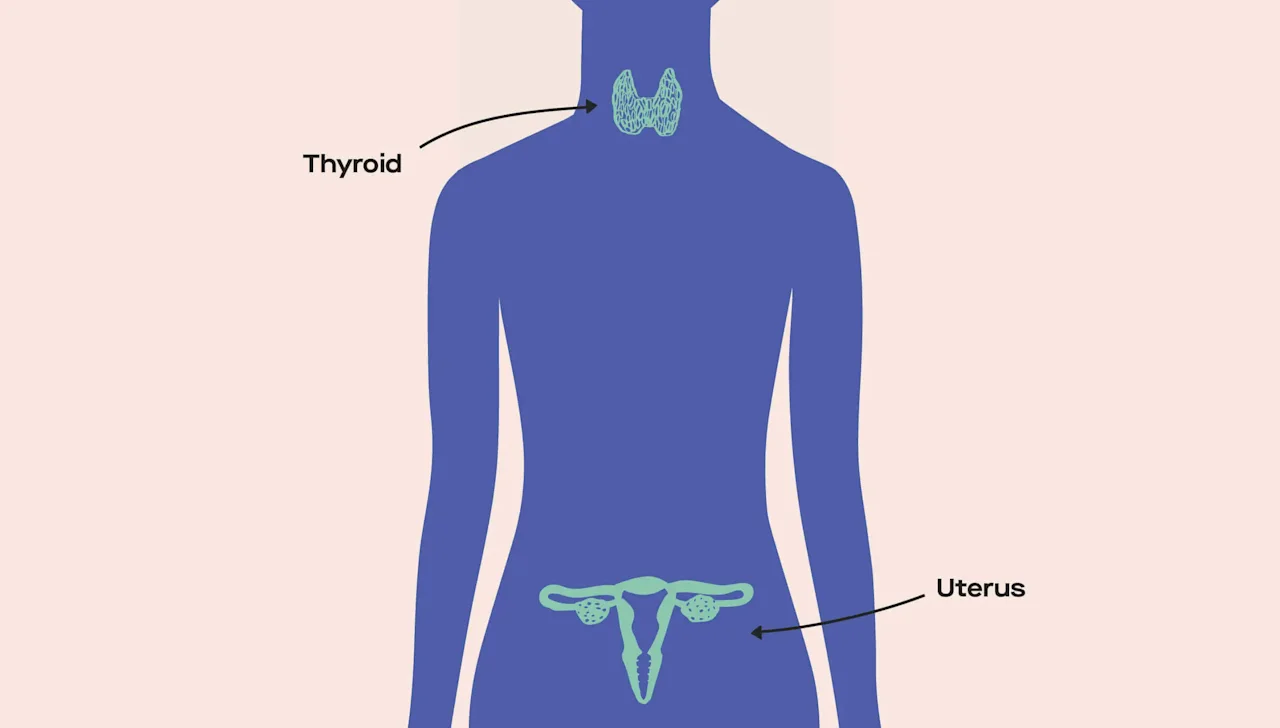
If your cycle lengths are getting shorter, if your flow has changed, if you discover frequently that your luteinizing hormone (LH) levels are always high while tracking your ovulation via ovulation tests — it can help you pinpoint other specific health issues. The hormones, like LH, that fluctuate and dictate the different points of your menstrual cycle require beautiful coordination between your ovaries, pituitary gland, and hypothalamus... and issues with your thyroid gland can interfere with that. These changes to your cycle can reveal conditions like polycystic ovary syndrome (PCOS), ovarian insufficiency, or thyroid disorders. Having this data is a great conversation starter with your doctor.When you track your cycle and ovulation patterns, you can also use information about your cycle to help doctors more effectively treat certain conditions like benign ovarian cysts (common, non-cancerous growths on your ovaries), painful intercourse, and general stomach pain.
“Benign ovarian cysts can form and often disappear on their own with the menstrual cycle,” Dr. Luo says. “Tracking symptoms of pain and bloating, and how they correlate with the menstrual cycle, [can help] clinicians in determining the best treatment options.”
4. To avoid pregnancy (though this is not endorsed by most physicians).
It may help some to conceive, but tracking your cycle and ovulation patterns has also been used to avoid pregnancy. Referred to as the rhythm method or the fertility awareness method, this kind of tracking uses ovulation tests, basal body temperature, or cervical mucus to determine when your “fertile window” occurs — as in the days when your body can actually conceive that month. Once you know when you’re ovulating, you can then figure out the best time to not get pregnant that month — allowing you to have sex and avoid conceiving.
The American College of Obstetricians and Gynecologists (ACOG) says that “fewer than 1–5 women out of 100 will become pregnant during the first year of perfect use” of the fertility awareness method, but with typical use, 12–24 women out of 100 will become pregnant — so proceed at your own risk.
If you’re using ovulation tests, you’ll be testing your urine and measuring the levels of LH present. LH is at its highest level before you start ovulating, so based on your test results, you can interpret whether you’ve entered your body’s fertile window in order to avoid unprotected sex. It’s important to note, though, that no ovulation tests are cleared by the FDA for contraceptive use.Modern Community member Mel D., 39, has successfully used the rhythm method to help her avoid getting pregnant. She started practicing it as a form of birth control after removing her IUD — specifically by tracking her ovulation with ovulation tests. Mel has found the rhythm method to be effective, as long as she is dedicated to tracking. “You need to be disciplined and keep your cycle at the top of your mind — just use [other forms of] protection if you're going to have sex during your fertile window.”
How to track your cycle and ovulation
There are lots of options for cycle and ovulation tracking:
Tracking apps: Period and ovulation tracking apps are a convenient way to track your cycle throughout the month. Apps count the number of days between the last day you reported being on your period and the first day you report being on your next period. Using that info, they can make a prediction of how long your cycle is and when your next period will come. Apps that allow you to track LH levels take the predictions to another level. If you're planning to use a tracking app to avoid pregnancy, make sure that the app is intended to be used that way — otherwise, unintended pregnancies may be more likely. Only some apps have been cleared by the FDA for contraceptive use and not without controversy.
Ovulation tests: Ovulation tests get a big thumbs-up from us. They involve the measurement of reproductive hormones (which we’re big fans of) and thus use actual biological indicators of ovulation to help you figure out where in your cycle you are. Ovulation tests overwhelmingly rely on measuring levels of LH in your urine to predict when you’ll ovulate and help you time sex or insemination around it. While most ovulation tests give you a negative/positive result based on LH averages, some detect LH at low, high, and peak levels — making it easier to track ovulation even if you don’t have “average” hormone levels.
Cervical mucus tracking: This requires you to pay attention to the mucus produced by your cervix throughout the month. Right before you ovulate, you’ll see more mucus than usual — specifically thin, slippery mucus, as explained by ACOG. Once you’re done ovulating, you will see less mucus, and any that you do see will be of a thicker consistency. If you’re avoiding pregnancy, you should use protection or avoid penetrative sex whenever you notice increased amounts of mucus.
Basal body temperature method (BBT): Another way of tracking ovulation, though ACOG warns you should only use this method if you are tracking ovulation for general health reasons — not if you are trying to avoid pregnancy — since it only reveals if ovulation has already happened. To measure your BBT (your body’s temperature when you're at rest), take your temperature every morning before you get out of bed or engage in any activity (that includes eating or drinking), and record it each time. ACOG explains that “the body’s normal temperature increases slightly during ovulation (0.5–1°F) and remains high until the end of the menstrual cycle,” and your fertile window is “the 2–3 days before this increase in temperature.”
There are many reasons why you might choose to use one cycle-tracking measure over another. For most of these methods, there are clear trade-offs in convenience and accuracy. Of frequently used methods, counting-based methods are the most convenient and require the least amount of effort, but are likely the least accurate. Cervical mucus monitoring takes more time and effort, but is more accurate in pinpointing the fertile window.
Generally speaking, the most accurate cycle-tracking measures will be the ones that measure ovulation most directly, such as measuring the hormones that are biologically implicated in ovulation (like LH). Ovulation tests track ovulation by measuring LH levels in urine.
The bottom line is this: Even if you’re not thinking about kids (right now or ever), tracking your cycle and ovulation can help you stay on top of your reproductive health — from better understanding your hormonal patterns to building awareness around your fertile window.
This article was reviewed by Dr. Jennifer Conti, MD, MS, MSc and Dr. Eva Marie Luo, MD.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.









