Here's what we'll cover
Here's what we'll cover
Even though most penile lumps and bumps are harmless, this is a part of the body you're probably—wisely—not accustomed to taking undue chances with. If you do spy a new lump or bump on your penis, there are ways to figure out what it is, why you may have it, and when you should ask a healthcare provider about it.
What can cause a lump on the penis?
There are many possible causes of lumps and bumps on your penis, and most of them are pretty harmless. Let’s look at some potential causes of that penis lump.
Moles on the penis
Moles are skin growths produced when your body generates too much pigment (melanin). They can appear anywhere on your body, including your penis. Most people have them, and on average individuals have anywhere from 15 to almost 40 moles (Cooke, 1985).
Moles are usually nothing to worry about—unless they grow in size, change in shape, color, or texture, have asymmetric or jagged borders, or bleed. Moles with any of these characteristics should be checked by a healthcare professional, as they could be a sign of skin cancer (melanoma). Fortunately, melanoma on the penis is rare (Jabiles, 2017; American Academy of Dermatology, n.d.).
Blemishes/zits
You can get a zit on any area of your body that has hair follicles—and that includes the penis. A zit on your penis is just like a zit on your face: sebum (oil), skin cells, dirt, or bacteria get trapped in a follicle, causing inflammation. Like typical acne, a penile zit can be a blackhead or a whitehead, which may contain fluid or pus.
The same ground rule applies here as with your face—popping a zit isn't recommended because it can lead to an infection. You don't want to use harsh acne creams on this sensitive area, either. Most zits in the groin or on the penis go away within a few days without needing special treatment. A zit on the penis that becomes more swollen or red instead of getting better might indicate that it’s infected.
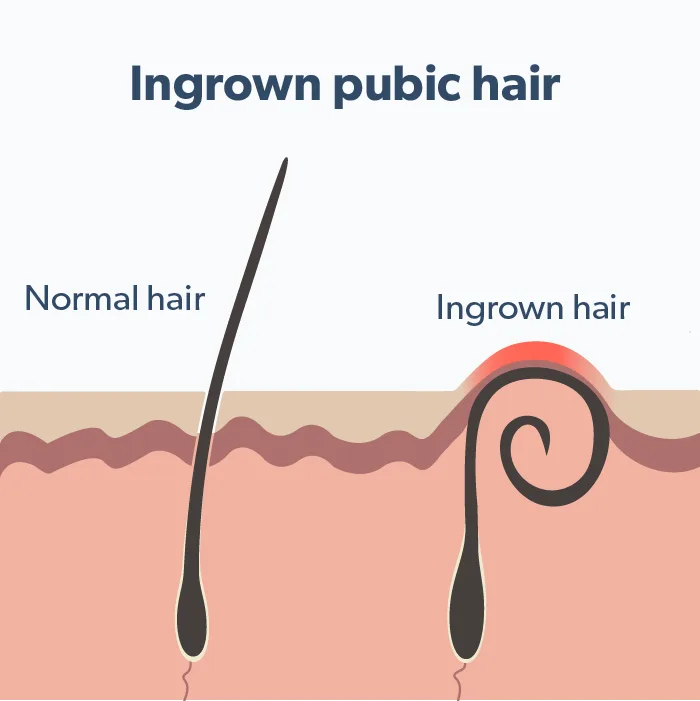
Ingrown hair
An ingrown hair occurs when a hair gets trapped under the skin instead of growing out of it.
This can cause a painful, itchy bump that may become irritated or filled with fluid or pus. Ingrown hairs are common in areas with shorter hair or hair that’s been recently shaved, like facial hair or pubic hair. Ingrown hairs might become infected and need to be extracted. It's a good idea to see a dermatologist or other healthcare provider instead of trying to remove them yourself, especially on a sensitive area like your penis.
An infected hair follicle can also be caused by folliculitis, a type of inflammation caused by a bacterial or fungal infection. If you have ingrown hairs on your penis or other parts of your body, a good first step is to stop shaving. If you stop shaving for a short period of time, the hairs may grow long enough to pull themselves out spontaneously, so the symptoms resolve on their own (Ogunbiyi, 2019).
Cysts
A cyst is a benign sac filled with fluid. It closely matches the color and texture of the skin around it. Cysts can develop on just about any part of your body, including your penis.
Cysts on the penis don’t usually look red or feel painful, though they may be sensitive. They typically don’t change shape, but they may get bigger.
Some sexually transmitted infections on the penis might look like cysts (more on that later). If you’re in doubt, your healthcare provider can help determine whether your bump is truly a cyst and advise you on any next steps.
Fordyce spots
Fordyce spots are enlarged oil or sebaceous glands that aren't associated with hair follicles. They look like small white spots or bumps (1 to 3 millimeters or .04 to .12 inches) on the lips, inside the mouth, and genitals. They're common, generally harmless, and don't require treatment (Singal, 2020).
Pearly penile papules
Say that one three times fast. The small flesh-colored bumps, also known as hirsutoid papillomas, are typically found on the head of the penis, where they encircle the entire penis head in a single or double row. They're benign, don't cause symptoms, and don't require treatment (American Urological Association, n.d.).
Angiokeratomas
Angiokeratomas of the penis are uncommon. These red bumps or lumps are made of enlarged blood vessels and can appear in small clusters in any body area. They may have a rough texture and thicken over time (Basu, 2018).
Angiokeratomas can indicate an underlying blood vessel condition like hypertension (high blood pressure) or varicocele (dilated veins in the scrotum), so it's a good idea to consult a healthcare provider if you notice them.
Peyronie's disease
Peyronie's disease is a condition in which fibrous scar tissue builds up in the penis, making it curve painfully or develop lumps. Peyronie's disease can worsen with time and may be associated with erectile dysfunction, so it's worth consulting a healthcare provider if you have those symptoms.
Lymphoceles
A lymphocele is a hard swelling that suddenly appears on the shaft under the skin after sex or masturbation. It happens when one of the lymph channels becomes temporarily blocked.
Lymph channels are part of our immune system; they move a liquid called lymph, which is rich in white blood cells—around the body to fight infection and quell inflammation. Lymphoceles usually go away on their own and don't require special treatment (Rane, 2013).
Molluscum contagiosum
This common, contagious, viral skin infection produces small, smooth, shiny bumps filled with a waxy substance. They can spread anywhere on the body via skin-to-skin contact. You can get molluscum contagiosum through close contact with someone who has it.
When it shows up on your penis, the chances are that you got it during sex. It usually goes away by itself, but it may take some time to do so (CDC, n.d.)
Sexually transmitted infections (STI)
A bump on the penis could also be the sign of an STI, such as:
Genital herpes: Genital herpes is caused by the herpes simplex virus (HSV-1 or HSV-2). It presents as small fluid-filled blisters that may be itchy or painful. A healthcare provider can prescribe antiviral medication to reduce or suppress outbreaks.
Genital warts: Genital warts are caused by human papillomavirus (HPV). These are painless growths or lumps around the penis, scrotum, foreskin, or anus. They may be flesh-colored, gray-white, pink-white, or brown. Warts may be single or in clusters and may be smooth and pearly or cauliflower-shaped. A healthcare provider can prescribe several medications and treatments to clear genital warts (Leung, 2018). In some cases, surgery may be necessary to remove them.
Syphilis: Caused by the Treponema pallidum bacterium, this STI usually presents as a firm, round, painless sore on the genitals. It's important to seek treatment for syphilis right away. If left untreated, syphilis may lead to severe health problems affecting the heart, brain, and other organs (CDC, 2017).
Scabies
Another condition that can cause bumps on the skin is scabies, in which tiny mites burrow under the surface of the skin and lay eggs. This can cause intense itching, especially at night.
Scabies is highly contagious but fairly easily treated with medication that kills the mites and their eggs.
Cancer
If you find a lump or bump on your penis, you may be worried about cancer. The fact is that cancer of the penis is exceedingly rare. Only about 2,200 men are diagnosed with penile cancer each year, representing less than 1% of all cancers (ACS, 2021-a).
Bumps from penile cancer usually don't hurt. The American Cancer Society recommends that you should see a healthcare provider about any new bump or abnormality on your penis, especially a bump that lasts for four weeks or longer or gets worse (ACS, 2021-b)
You should also see a healthcare provider if you notice a bump on your penis after unprotected sexual contact or if you have any of the following symptoms: pain during sex or an erection, burning when you urinate, open sores, itchy or painful blisters, fever, fatigue, or an unusually colored or bad-smelling discharge. Or, just see a healthcare provider if you're worried—reassurance in and of itself can be helpful.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
American Academy of Dermatology (AAD). (n.d.). Moles: Who gets and types . Retrieved Aug. 23, 2020 from https://www.aad.org/public/diseases/a-z/moles-types
American Cancer Society (ACS-a). (2021). Key Statistics for Penile Cancer . Retrieved Dec. 8, 2021, from https://www.cancer.org/cancer/penile-cancer/about/key-statistics.html
American Cancer Society (ACS-b). (2021). Signs and Symptoms of Penile Cancer: Signs Of Penile Cance r. Retrieved Dec. 8, 2021 from https://www.cancer.org/cancer/penile-cancer/detection-diagnosis-staging/signs-symptoms.html
American Urological Association (AUA). (n.d.). Pearly Penile Papules. Retrieved from https://www.auanet.org/education/auauniversity/education-products-and-resources/pathology-for-urologists/penis/inflammatory-and-tumor-like-lesions/pearly-penile-papules
Basu, P. (2018). Penile Angiokeratoma (Peaker): A Distinctive Subtype of Genital Angiokeratoma. Cureus , 10 (12). doi: 10.7759/cureus.3793. Retrieved from https://pubmed.ncbi.nlm.nih.gov/30868007/
Centers for Disease Control & Prevention (CDC). (2017). STD Facts - Syphilis . Retrieved Aug. 2, 2020 from https://www.cdc.gov/std/syphilis/stdfact-syphilis.htm
Cooke, K. R., Spears, G. F., & Skegg, D. C. (1985). Frequency of moles in a defined population. Journal of Epidemiology and Community Health , 39 (1), 48–52. doi:10.1136/jech.39.1.48. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1052400/
Jabiles, A. G. (2017). Penile melanoma: a 20-Year analysis of six patients at the National Cancer Institute of Peru, Lima. Ecancermedicalscience, 11 , 731. doi: 10.3332/ecancer.2017.731. Retrieved from: https://pubmed.ncbi.nlm.nih.gov/28487750/
Lee, J. H., Lee, J. H., Kwon, N. H., Yu, D. S., Kim, G. M., Park, C. J., et al (2012). Clinicopathologic Manifestations of Patients with Fordyce's Spots. Annals of Dermatology , 24 (1), 103–106. doi: 10.5021/ad.2012.24.1.103. Retrieved from https://anndermatol.org/DOIx.php?id=10.5021/ad.2012.24.1.103
Leung, A. K., Barankin, B., Leong, K. F., & Hon, K. L. (2018). Penile warts: an update on their evaluation and management. Drugs In Context , 7 , 212563. doi: 10.7573/dic.212563. Retrieved from https://www.drugsincontext.com/penile-warts-an-update-on-their-evaluation-and-management/
National Health Service (NHS). (n.d.) Common health questions: What is this lump on my penis? Retrieved Aug. 2, 2020 from https://www.nhs.uk/common-health-questions/mens-health/what-is-this-lump-on-my-penis/
Ogunbiyi, A. (2019). Pseudofolliculitis barbae; current treatment options. Clinical, Cosmetic and Investigational Dermatology, 12 , 241–247. doi: 10.2147/CCID.S149250 Retrieved from https://pubmed.ncbi.nlm.nih.gov/31354326/
Rane, V. (2013). Penile appearance, lumps and bumps. Australian Family Physician , 42 (5), 270–274. Retrieved from https://pubmed.ncbi.nlm.nih.gov/23781523/
Singal, A., Kaur, I., & Jakhar, D. (2020). Fox-Fordyce Disease: Dermoscopic Perspective. Skin Appendage Disorders , 6 (4), 247–249. doi:10.1159/000508201. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7445575/










