Here's what we'll cover
Here's what we'll cover
Here's what we'll cover
Magnesium is an essential mineral that is abundant in your body and is needed for proper functioning. Magnesium is involved in over 300 different metabolic pathways, such as making proteins, blood glucose control, and blood pressure regulation (NIH, 2019). It is also involved in energy production, the creation of DNA, and plays an important role in muscle contraction. Low levels of magnesium have been associated with health problems like high blood pressure, high cholesterol, type 2 diabetes, coronary artery disease, and sudden cardiac death.
A healthy adult has approximately 25 grams of magnesium in their body; 50–60% is kept in your bones, while most of the rest of it is in your soft tissues (NIH, 2019). A small amount of magnesium, less than 1%, is circulating in your blood. Despite being such an essential element, studies show that a significant proportion of Americans do not get enough magnesium in their diets (Schwalfenberg, 2017).
Unfortunately, testing for magnesium levels is difficult. The 1% of your magnesium that floats around in your bloodstream is the only magnesium level we can test, called the serum magnesium level. However, it is tightly regulated so that whenever your blood levels decrease, your body releases magnesium from the bones and muscles.
So you can have very little magnesium in your body, but still have normal serum levels of magnesium, making blood tests for this micronutrient not very reliable. Most healthcare providers rely on a combination of lab tests and clinical assessments to get an accurate idea of what your magnesium levels are and if you need supplementation.
How does magnesium affect your heart health?
Normal magnesium levels may benefit the heart and cardiovascular system in several ways:
Keeps the heart pumping regularly
Muscle cells in your heart and blood vessels have ion transport channels that move ions like sodium, potassium, and calcium into and out of cells, causing muscle contractions (Severino, 2019). Magnesium is necessary for this ion pump to work and helps keep the heart pumping with a regular rhythm; magnesium deficiency leads to abnormal heart rhythms (arrhythmias), which can sometimes be fatal.
May help decrease blood pressure
Magnesium competes with calcium for many of the same ion transport channels; a magnesium deficiency leads to a buildup of calcium, which in turn causes spasms of the heart and blood vessels and can result in elevated blood pressures. The presence of magnesium decreases the amount of calcium in the cells and allows the heart and blood vessels to relax, thereby potentially reducing blood pressure. One study showed a small decrease in blood pressure in people taking magnesium (an average of 368 mg/day). However, magnesium supplementation is not considered standard high blood pressure treatment; more studies are needed to better understand the role of magnesium in managing blood pressure (Zhang, 2016).
May decrease the risk of type 2 diabetes
Magnesium helps the pancreas release insulin and move glucose out of the bloodstream, thereby keeping the overall amount of glucose in the blood under control (Severino, 2019). Diets with higher levels of magnesium have a lower risk of type 2 diabetes (NIH, 2019). However, according to the American Diabetes Association, there is not enough evidence to recommend the routine use of magnesium supplementation to improve blood sugar control in people with type 2 diabetes (Evert, 2013). Diabetes is a known risk factor for heart disease.
May decrease the risk of heart disease (cardiovascular disease)
There are several different ways that magnesium may reduce the risk of heart disease. One pathway is via its antioxidant and anti-inflammatory effects; a magnesium deficiency increases inflammation and damage to blood vessel walls, along with cholesterol deposits (atherosclerosis) in the coronary blood vessels. All of these changes increase your risk of a heart attack or stroke. Another way that magnesium may protect your heart is by decreasing the ability of platelets to clump up and form a clot, as happens in a heart attack or stroke. Magnesium deficiency is associated with an increased risk of heart disease and heart attacks (Severino, 2019).
Additional health benefits of magnesium
In addition to all of the ways that magnesium can potentially improve your heart health, it can also have beneficial effects in other conditions.
Migraines
Studies show that some people who suffer from migraines have low magnesium levels (Gröber, 2015). However, the exact role that magnesium plays in migraines is not well understood. Magnesium affects some of the receptors in the brain pathways that can lead to headaches, like serotonin and N-methyl-D-aspartate (NMDA) receptors. One study shows an improvement in migraine symptoms and a trend towards decreasing migraine frequency with magnesium supplementation, although this trend was not statistically significant (Gaul, 2015). While it is not considered the mainstay of migraine treatment, the Academy of Neurology and American Headache Society state that magnesium supplementation is “probably effective” for migraine prevention (Holland, 2012).
Sleep
Sleep problems are widespread, especially as we get older. The brain chemicals (neurotransmitters) NMDA and gamma-aminobutyric acid (GABA) play an important role in sleep regulation, and both of these neurotransmitters interact with magnesium. How magnesium affects sleep is unclear; however, one trial showed that people taking magnesium supplements subjectively reported falling asleep faster and staying asleep longer (Abbasi, 2012). More research needs to be done in this area.
Depression
Since magnesium affects brain chemistry (through neurotransmitters), it may also help improve depression symptoms. Studies have shown an association between magnesium deficiency and depression, and several show an improvement in depression after taking magnesium supplements. However, others show no benefit. More information is needed to better understand how magnesium and depression are related (Wang, 2018).
Osteoporosis
Magnesium interacts with bone cells and affects the balance of creating new bone versus removing old bone. Studies have found that women with osteoporosis have lower magnesium levels than those without osteoporosis (NIH, 2019). One small study even found that a group of postmenopausal women who took magnesium supplements (290 mg/day) had decreased bone turnover, which translates to reduced bone loss (Aydin, 2010). It is clear that magnesium promotes bone health, but its role in preventing and treating osteoporosis needs to be explored further.
How to get magnesium
Dietary surveys of Americans have shown that overall, approximately 50% of people aged 19–50 years don’t get their estimated average requirement of magnesium from their food; this number climbs to 70–80% if you focus on people over 71 years old (Moshfegh, 2009).
The recommended dietary allowance (RDA) is 400–420 mg/day for men and 310–320 mg/day for women (NIH, 2019). Where can you get magnesium? It is in many different foods—especially green leafy vegetables (like spinach), legumes, nuts, seeds, and whole grains. Most foods that are high in fiber also have high levels of magnesium as do fortified foods, like breakfast cereal, and bottled water.
Here is a list of some magnesium-rich foods (NIH, 2019):
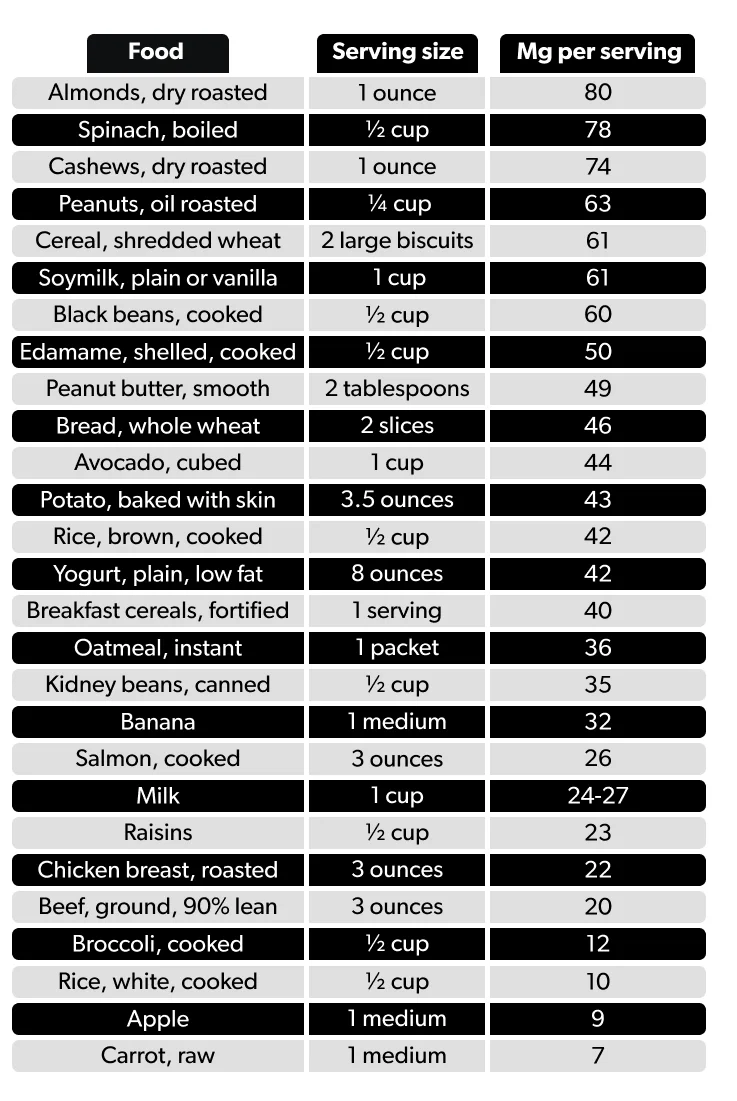
If you are not able to get enough magnesium from your diet, you can turn to supplements. Magnesium in supplements comes in several forms: magnesium aspartate, magnesium carbonate, magnesium chloride, magnesium lactate, magnesium oxide, magnesium sulfate, and magnesium citrate. Some studies have shown that the absorption of the aspartate, citrate, lactate, and chloride forms are better than the oxide and sulfate formulations (NIH, 2019).
Side effects/potential risks of magnesium
Even though most Americans do not eat enough magnesium, healthy people generally don’t get symptoms from low magnesium; this is because the kidneys limit how much magnesium gets excreted in the urine when levels are low. However, people with medical conditions like Crohn’s disease, alcoholism, type 2 diabetes, and older adults can have a magnesium deficiency (hypomagnesemia). Hypomagnesemia can cause a loss of appetite, nausea, vomiting, fatigue, and weakness in the early stages (NIH, 2019). As this condition worsens, you can develop numbness, tingling, muscle cramps, seizures, and irregular heart rhythms.
Likewise, too much magnesium can be harmful as well. Again, since the kidneys manage how much magnesium is removed in the urine, most healthy people can excrete the excess magnesium from their diet. However, if you have impaired kidney function or take too much supplemental magnesium, you can accumulate unhealthy levels of magnesium; this leads to diarrhea, nausea, and abdominal cramping. Some antacids and laxative contain very high doses (more than 5,000 mg) and have been associated with magnesium toxicity, which can cause the following symptoms (NIH, 2019):
Low blood pressure
Nausea/vomiting
Facial flushing
Difficulty urinating (urinary retention)
Lethargy
Muscle weakness
Irregular heartbeat
Death
Before starting magnesium supplements, talk to your healthcare provider about other medicines you are taking; magnesium interacts with several types of medications, and this can potentially affect the ability of the drug to work or change your magnesium levels. Some of the medicines that interact with magnesium supplements include (NIH, 2019):
Bisphosphonates (e.g., alendronate, risedronate)
Bisphosphonates (e.g., alendronate, risedronate): These drugs are typically used to treat osteoporosis; magnesium supplements can decrease their absorption. Bisphosphonates and magnesium should be taken at least two hours apart from each other to avoid this interaction.
Quinolone antibiotics and tetracycline antibiotics
Quinolone antibiotics (e.g., ciprofloxacin, levofloxacin) and tetracycline antibiotics (e.g., tetracycline, doxycycline): Taking these drugs with magnesium makes them less absorbable in your gut, and thereby less effective at treating your infection. To avoid this, take the antibiotic at least two hours before or at least four to six hours after your magnesium supplement.
Loop diuretics and thiazide diuretics
Loop diuretics (e.g., bumetanide, furosemide), thiazide diuretics (e.g., hydrochlorothiazide): Diuretics, also known as “water pills,” are typically used to treat high blood pressure and heart failure. Taking them may cause the body to excrete too much magnesium in the urine, which can decrease the levels of magnesium in the body. Know the symptoms of magnesium deficiency and alert your healthcare provider if you start to experience any of them; early recognition may help prevent health problems.
Potassium-sparing diuretics
Potassium-sparing diuretics (e.g., amiloride, spironolactone): Unlike the other diuretics, this type decreases the amount of magnesium removed in the urine and can potentially cause an excess of magnesium. Talk to your provider if you have any symptoms of high magnesium.
Proton pump inhibitors
Proton pump inhibitors (PPIs) (e.g., omeprazole, pantoprazole) are used to treat heartburn or acid reflux. Using PPIs for more than a year can lead to low magnesium levels. Your provider may check your magnesium levels before starting a PPI and then monitor them periodically while you are on the medication.
In conclusion
Although magnesium affects many aspects of your health, you should strive to get most of your magnesium from your diet. A diet with a variety of fruits, vegetables, whole grains, nuts, etc. is ideal. If you need to supplement your diet with magnesium pills, be sure to discuss your options with your healthcare provider to avoid any adverse effects.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
References
Abbasi, B., Kimiagar, M., Sadeghniiat, K., Shirazi, M. M., Hedayati, M., & Rashidkhani, B. (2012). The effect of magnesium supplementation on primary insomnia in elderly: A double-blind placebo-controlled clinical trial. Journal of Research in Medical Sciences , 17 (12), 1161–1169. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/23853635
Aydın, H., Deyneli, O., Yavuz, D., Gözü, H., Mutlu, N., Kaygusuz, I., et al. (2010). Short-Term Oral Magnesium Supplementation Suppresses Bone Turnover in Postmenopausal Osteoporotic Women. Biological Trace Element Research , 133 (2), 136–143. doi: 10.1007/s12011-009-8416-8. Retrieved from https://pubmed.ncbi.nlm.nih.gov/19488681/
Gaul, C., Diener, H.-C., & Danesch, U. (2015). Improvement of migraine symptoms with a proprietary supplement containing riboflavin, magnesium and Q10: a randomized, placebo-controlled, double-blind, multicenter trial. The Journal of Headache and Pain , 16 (1), 32. doi: 10.1186/s10194-015-0516-6. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4393401/
Gröber, U., Schmidt, J., & Kisters, K. (2015). Magnesium in Prevention and Therapy. Nutrients , 7 (9), 8199–8226. doi: 10.3390/nu7095388. Retrieved from https://pubmed.ncbi.nlm.nih.gov/26404370/
Holland, S., Silberstein, S., Freitag, F., Dodick, D., Argoff, C., & Ashman, E. (2012). Evidence-based guideline update: NSAIDs and other complementary treatments for episodic migraine prevention in adults: [RETIRED]. Neurology , 78 (17), 1346–1353. doi: 10.1212/wnl.0b013e3182535d0c. Retrieved from https://pubmed.ncbi.nlm.nih.gov/22529203/
Moshfegh, A., Goldman, J., Ahuja, J., Rhodes, D., & LaComb, R. (2009). What We Eat In America, NHANES 2005-2006: Usual Nutrient Intakes from Food and Water Compared to 1997 Dietary Reference Intakes for Vitamin D, Calcium, Phosphorus, and Magnesium. U.S. Department of Agriculture, Agricultural Research Service . Retrieved from https://www.ars.usda.gov/ARSUserFiles/80400530/pdf/0506/usual_nutrient_intake_vitD_ca_phos_mg_2005-06.pdf
National Institutes of Health (NIH). (2019, October 11). Office of Dietary Supplements - Magnesium. Retrieved Nov. 10, 2019 from https://ods.od.nih.gov/factsheets/Magnesium-HealthProfessional/
Schwalfenberg, G. K. & Genuis, S. J. (2017). The Importance of Magnesium in Clinical Healthcare. Scientifica , 2017 , 1–14. doi: 10.1155/2017/4179326. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5637834/
Severino, P., Netti, L., Mariani, M. V., Maraone, A., D’Amato, A., Scarpati, R., et al. (2019). Prevention of Cardiovascular Disease: Screening for Magnesium Deficiency. Cardiology Research and Practice , 2019 , 1–10. doi: 10.1155/2019/4874921. Retrieved from https://www.hindawi.com/journals/crp/2019/4874921/
Wang, J., Um, P., Dickerman, B., & Liu, J. (2018). Zinc, Magnesium, Selenium and Depression: A Review of the Evidence, Potential Mechanisms and Implications. Nutrients , 10 (5), 584. doi: 10.3390/nu1005058410. Retrieved from https://pubmed.ncbi.nlm.nih.gov/29747386/









