Here's what we'll cover
Here's what we'll cover
A rash on your breast can be bothersome. If it’s itchy, or painful, it can even keep you from being able to function on a day-to-day basis. Rashes can be caused by many things, from something as innocuous as an insect bite to an infection from breastfeeding, and in rare cases, even something more serious, like breast cancer.
If you’ve spotted a new rash on your breast, the first step is understanding what triggered it. Here are a few possible causes of breast rashes and common treatment options for each.
What is a breast rash?
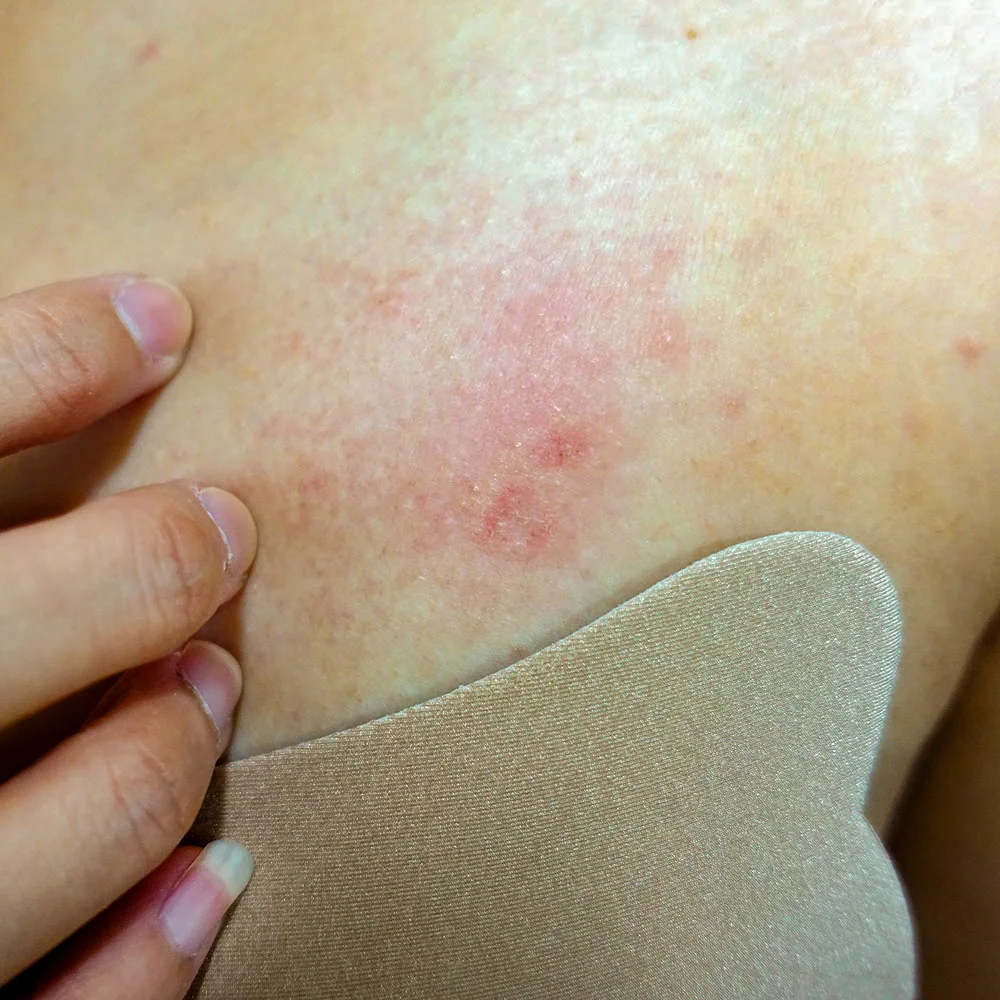
Breast rashes describe any new redness or skin irritation on your breast. It can look very different depending on the cause, and the appearance can also vary from person to person.
Signs of a breast rash may include skin that is:
Red or discolored
Inflamed
Irritated
Itchy
Scaly
Blistery
Painful
Raised or bumpy
Oozing or swollen
Some people may also experience discharge from their nipples of clear, white, or bloody fluid. Some may also have additional symptoms, like fever or swollen lymph nodes in their underarms.
Possible causes of a breast rash
Often a breast rash is linked to an underlying skin condition that can affect any part of the body. For example, eczema can crop up on the inside of your elbows or on your nipples. Acne most commonly appears on the face but is common on the back and chest areas too. If one of the following conditions is something you’ve been diagnosed with already, it may be worth going over your medical history with a healthcare provider and showing them your rash to see if this might be the cause:
Skin conditions
Up to 1 in 10 adults have eczema, or atopic dermatitis. It’s typically more common in childhood but can continue into adulthood too. Eczema is a chronic skin condition that causes dry, itchy skin. A rash can develop if you scratch or rub it (Nemeth, 2021).
Seborrheic dermatitis is another chronic skin condition that can cause a rash. The skin may have a greasy or oily quality to it since this type of dermatitis affects areas of the body that have sebaceous (oil-producing) glands. Rashes may appear on your scalp, chest, under the breast, groin, or belly button (Ely, 2010).
Psoriasis, a chronic inflammatory condition that causes thick rashes with an oval or round shape, affects about one in every 50 people (Kim, 2017). Rashes may also be accompanied by silvery scales called plaques that sometimes feel painful or itchy. Plaques commonly appear around the joints, scalp, torso, and butt but can show up anywhere on your body (Ely, 2010).
Psoriasis and eczema flare-ups are managed through topical treatments like corticosteroids. In the case of eczema, your healthcare provider may recommend a specialized ointment and daily moisturizing routine (Kim, 2017; Nemeth, 2021).
Allergic reaction
Allergic reactions can cause a rash. This could be anything from an insect bite or sting to something your skin came in contact with like food, plants, clothing, a new laundry detergent, soap, or lotion––to name a few.
An allergy can also present as contact dermatitis, which appears as a red rash or blisters. You may also notice hives, which are bumps on your skin that become red and itchy.
If you have a rash due to an allergic reaction, stop using all creams, detergents, soaps, and deodorants that might be irritating your skin. You can then add them back one at a time to determine the culprit. If you can’t figure out the source, visit a healthcare provider for further evaluation. They can prescribe topical ointments and antihistamine medications may be prescribed if you have a rash from an allergic reaction.
Breastfeeding
People who are breastfeeding might develop cracking, peeling, dryness, or infection in the skin on their nipples, areolas (the area around the nipple), dermatitis, or eczema on their nipples or areolas due to trapped moisture, bacteria, or irritation from nursing or pumping. Nipple eczema presents as a dry, scaly, or moist rash that may ooze. You may also feel a burning or painful sensation while nursing (Heller, 2012).
Mastitis is a condition where breast tissue becomes inflamed or infected, and it may cause redness, warmth, or swelling in the skin over the affected area. You may also experience a fever or chills. As many as 1 in 5 women experience mastitis while breastfeeding (Pevzner, 2020).
Left untreated, mastitis may develop into an abscess. Breast abscesses can cause pain, redness, swelling, and you may notice a lump in your breast. It can also be accompanied by fever. The chances of developing a breast abscess are higher during the first month of breastfeeding when a baby begins teething and while weaning, but it can happen at any point (Kataria, 2013).
For mastitis, topical antifungal medications, antibiotics, and pain relievers (like ibuprofen) are often used. If you’ve developed an abscess, you can visit your healthcare provider for treatment, which may include draining the abscess and then oral antibiotics (Kataria, 2013; Pevzner, 2020).
Heat rash or chafing
If you live somewhere hot and humid and spend a lot of time outside in the summer, you could develop a rash from the heat.
Heat rash, also called miliaria rubra, is distinguished by a reddish or pinkish hue. It occurs when sweat pores become blocked, so you may be more likely to find it in parts covered up by clothing, such as where your bra sits against your skin.
A similar reaction can occur in areas between skin that rub against each other, such as the area under your breast. This is called intertrigo and often results from moisture being trapped in the folds of skin and chafing between those areas.
Heat rash and intertrigo typically resolve on their own when you let the affected areas air out. Some people find that putting a small amount of petroleum jelly on an area affected by intertrigo can help alleviate chafing. Wear loose clothing and breathable fabrics when you’re in hot or humid conditions, and change out of clothes after things like working out or swimming. If you notice severe swelling or oozing from the area, speak with a healthcare professional.
Bacterial and fungal infections
Tinea corporis, more commonly known as ringworm, is not a worm at all but rather a type of fungal infection. Ringworm is characterized by a red, scaly rash with a ring around it––hence the name. It’s caused by a fungus that feeds on keratin, a protein found in the skin, hair, and nails. Ringworm can affect any part of the skin, including the breasts.
Like other fungal infections, heat, humidity, and tight clothing create hospitable conditions for ringworm (Yee, 2021). Treatment typically involves the use of topical antifungal cream or corticosteroids.
Scabies
Scabies looks like a rash but is actually a condition caused by tiny mites that burrow into the skin, creating small, red pimples or bumps. You may also observe rows of these where mites have laid their eggs.
The mites that cause scabies prefer areas of the body with skin folds like in between fingers, and elbows, but they can appear anywhere on the body.
Luckily, there are effective medications for treating scabies. It’s also important to thoroughly clean all bedsheets and areas where the mites could remain to prevent reinfection.
Viral conditions
A breast rash can also be a symptom of a viral condition like measles, chickenpox, or shingles, but the rash typically isn’t limited to the breast area and usually extends to other areas of the body. Also, measles and chickenpox are unlikely in adults—especially if you’re vaccinated. Shingles is caused by the same virus (herpes zoster) as chickenpox but only occurs in people who have had a previous bout of chickenpox. It’s more common in older adults and can cause skin rashes that are extremely painful (Johnson, 2015).
The rash typically appears as a band that wraps around one section of the torso, but can affect any area of the body. Treatment is typically supportive and adults should get vaccine booster shots every 10 years in order to prevent shingles.
Breast conditions
Some conditions––including certain types of breast cancer––can appear with a rash on the breast. This is a rare occurrence.
Inflammatory breast cancer: A rare but aggressive form of breast cancer, symptoms include rash, redness, swelling, thickening, and peau d’orange (pitting of the skin that resembles an orange peel) (Yamauchi, 2012).
Paget’s diseaseThis represents 1–3% of all breast cancers. The salient symptom is a scaly, red rash either on the nipple or next to it (Liu, 2015).
If the skin on your breast is rough or resembles the skin of an orange with dimpling, or if you’re experiencing pain in your breast or blood discharge from your nipple, it’s a good idea to visit a healthcare provider.
A mammogram or biopsy may be ordered to help your healthcare provider make a diagnosis (Yamauchi, 2012).
When to see a healthcare provider
Many rashes go away on their own. However, if you have a breast rash that’s new and doesn’t go away, it’s a good idea to consult with a healthcare provider. A trip to the doctor may also be warranted if you notice any of the following:
Discharge from nipples, especially bloody discharge
A rash that is painful or has open sores
Other breast changes such as swelling, increase in size, tenderness, or lumps that don’t fluctuate with your menstrual cycle
Additional symptoms like a high fever or swollen lymph nodes in your underarms.
If you’ve noticed a rash on your breast, make an appointment with a health professional. They can help you understand the cause and recommend the appropriate treatment.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
Ely, J. W. & Seabury Stone, M. (2010). The generalized rash: part I. Differential diagnosis. American Family Physician, 81 (6), 726–734. Retrieved from https://pubmed.ncbi.nlm.nih.gov/20229971/
Hamwi, M. W. & Winters, R. (2021). Mammary Duct Ectasia. [Updated Dec 29, 2021]. In StatPearls . StatPearls Publishing. Retrieved from https://pubmed.ncbi.nlm.nih.gov/32491597/
Heller, M. M., Fullerton-Stone, H., & Murase, J. E. (2012). Caring for new mothers: diagnosis, management and treatment of nipple dermatitis in breastfeeding mothers. International Journal of Dermatology, 51 (10), 1149–1161. doi: 10.1111/j.1365-4632.2011.05445.x. Retrieved from https://pubmed.ncbi.nlm.nih.gov/22994661/
Johnson, R. W., Alvarez-Pasquin, M. J., Bijl, M., Franco, E., Gaillat, J., Clara, J. G., et al. (2015). Herpes zoster epidemiology, management, and disease and economic burden in Europe: a multidisciplinary perspective. Therapeutic Advances in Vaccines, 3 (4), 109–120. doi: 10.1177/2051013615599151. Retrieved from https://pubmed.ncbi.nlm.nih.gov/26478818/
Kataria, K., Srivastava, A., & Dhar, A. (2013). Management of lactational mastitis and breast abscesses: review of current knowledge and practice. The Indian Journal of Surgery, 75 (6), 430–435. doi: 10.1007/s12262-012-0776-1. Retrieved from https://pubmed.ncbi.nlm.nih.gov/24465097/
Kim, W. B., Jerome, D., & Yeung, J. (2017). Diagnosis and management of psoriasis. Canadian Family Physician, 63 (4), 278–285. Retrieved from https://pubmed.ncbi.nlm.nih.gov/28404701/
Liu, J., Zhao, Z., Zhou, J., & Zhang, J. (2015). An unusual presentation of Paget's disease of the nipple in a young woman: a case report. International Journal of Clinical and Experimental Medicine, 8 (3), 4694–4696. Retrieved from https://pubmed.ncbi.nlm.nih.gov/26064405/
Metin, A., Dilek, N., & Bilgili, S. G. (2018). Recurrent candidal intertrigo: challenges and solutions. Clinical, Cosmetic and Investigational Dermatology, 11, 175–185. doi: 10.2147/CCID.S127841. Retrieved from https://pubmed.ncbi.nlm.nih.gov/29713190/
Nemeth, V., & Evans, J. (2021). Eczema. [Updated Aug 11, 2021]. In StatPearls . StatPearls Publishing. Retrieved from https://pubmed.ncbi.nlm.nih.gov/30855797/
Pevzner, M. & Dahan, A. (2020). Mastitis while breastfeeding: Prevention, the importance of proper treatment, and potential complications. Journal of Clinical Medicine, 9 (8), 2328. doi: 10.3390/jcm9082328. Retrieved from https://pubmed.ncbi.nlm.nih.gov/32707832/
Yamauchi, H., Woodward, W. A., Valero, V., Alvarez, R. H., Lucci, A., Buchholz, T. A., et al. (2012). Inflammatory breast cancer: what we know and what we need to learn. The Oncologist, 17 (7), 891–899. doi: 10.1634/theoncologist.2012-0039. Retrieved from https://pubmed.ncbi.nlm.nih.gov/22584436/